MY HEALTH AIYIN
MY HEALTH AIYIN
Medical Billing Business Proposal
Medical Billing Business Proposal
Medical Billing Business Proposal
Medical Billing Business Proposal
Presented By
HTML5/CSS3 Mastery
Product Design
Branding
Collaborative Team Player
Presented By
HTML5/CSS3 Mastery
Product Design
Branding
Collaborative Team Player
Presented By
HTML5/CSS3 Mastery
Product Design
Branding
Collaborative Team Player
Presented By
HTML5/CSS3 Mastery
Product Design
Branding
Collaborative Team Player










Many Happy Clients



Many Happy Clients



Many Happy Clients
























Sequence
01.
Executive Summary
02.
Introduction to an Ideal Billing Company
03.
Organizational Structure, Workflow, and Strategic Goals
04.
Services
05.
Targeted Specialties
06.
Tools and Technologies
07.
Revenue Cycle Lifecycle
08.
Common Challenges in Medical Billing
09.
Benefits of Outsourcing Medical Billing
10.
Target Market Analysis
11.
Cost-Benefit Analysis
12.
Pricing Strategy
13
Financial Dashboard
14.
Call to Action
15.
References
01
Executive Summary
01
Executive Summary
01
Executive Summary

Expected Financial Outcome :
. At My Health Aiyin, we specialize in simplifying medical billing to help healthcare providers focus on delivering exceptional patient care. By managing financial complexities with precision, we ensure seamless and efficient billing processes tailored to your practice's needs.
. Our approach is guided by core values of accuracy, integrity, and transparency. We streamline workflows, reduce administrative burdens, and uphold the highest standards of professionalism to build trust and reliability with our clients.
. With a vision of leading the industry in innovative billing solutions, we aim to redefine financial management for healthcare practices. Let us handle the details so you can prioritize what truly matters—your patients.

Our company will target :
. Small and solo practices, an underserved segment with high outsourcing potential.
. Strategic states like California, Texas, and New York.
. Leverage operational cost advantages as compared to Market without compromising to deliver high-quality, affordable billing services.

Introduction :
The U.S. medical billing services market, valued at $5.7 billion in 2023, is projected to grow at a CAGR of 11.78%, reaching $12.26 billion by 2030 (Grand View Research). Key growth drivers include:
Increasing regulatory complexities, requiring outsourced billing solutions.
Adoption of cloud-based systems and AI-driven tools.
Rising trend of outsourcing by small to mid-sized practices to reduce costs and administrative burdens.
Expected Financial Outcome :
. At My Health Aiyin, we specialize in simplifying medical billing to help healthcare providers focus on delivering exceptional patient care. By managing financial complexities with precision, we ensure seamless and efficient billing processes tailored to your practice's needs.
. Our approach is guided by core values of accuracy, integrity, and transparency. We streamline workflows, reduce administrative burdens, and uphold the highest standards of professionalism to build trust and reliability with our clients.
. With a vision of leading the industry in innovative billing solutions, we aim to redefine financial management for healthcare practices. Let us handle the details so you can prioritize what truly matters—your patients.
Our company will target :
. Small and solo practices, an underserved segment with high outsourcing potential.
. Strategic states like California, Texas, and New York.
. Leverage operational cost advantages as compared to Market without compromising to deliver high-quality, affordable billing services.
Introduction :
The U.S. medical billing services market, valued at $5.7 billion in 2023, is projected to grow at a CAGR of 11.78%, reaching $12.26 billion by 2030 (Grand View Research). Key growth drivers include:
Increasing regulatory complexities, requiring outsourced billing solutions.
Adoption of cloud-based systems and AI-driven tools.
Rising trend of outsourcing by small to mid-sized practices to reduce costs and administrative burdens.
Expected Financial Outcome :
. At My Health Aiyin, we specialize in simplifying medical billing to help healthcare providers focus on delivering exceptional patient care. By managing financial complexities with precision, we ensure seamless and efficient billing processes tailored to your practice's needs.
. Our approach is guided by core values of accuracy, integrity, and transparency. We streamline workflows, reduce administrative burdens, and uphold the highest standards of professionalism to build trust and reliability with our clients.
. With a vision of leading the industry in innovative billing solutions, we aim to redefine financial management for healthcare practices. Let us handle the details so you can prioritize what truly matters—your patients.
Our company will target :
. Small and solo practices, an underserved segment with high outsourcing potential.
. Strategic states like California, Texas, and New York.
. Leverage operational cost advantages as compared to Market without compromising to deliver high-quality, affordable billing services.
Introduction :
The U.S. medical billing services market, valued at $5.7 billion in 2023, is projected to grow at a CAGR of 11.78%, reaching $12.26 billion by 2030 (Grand View Research). Key growth drivers include:
Increasing regulatory complexities, requiring outsourced billing solutions.
Adoption of cloud-based systems and AI-driven tools.
Rising trend of outsourcing by small to mid-sized practices to reduce costs and administrative burdens.
Expected Financial Outcome :
. At My Health Aiyin, we specialize in simplifying medical billing to help healthcare providers focus on delivering exceptional patient care. By managing financial complexities with precision, we ensure seamless and efficient billing processes tailored to your practice's needs.
. Our approach is guided by core values of accuracy, integrity, and transparency. We streamline workflows, reduce administrative burdens, and uphold the highest standards of professionalism to build trust and reliability with our clients.
. With a vision of leading the industry in innovative billing solutions, we aim to redefine financial management for healthcare practices. Let us handle the details so you can prioritize what truly matters—your patients.
Our company will target :
. Small and solo practices, an underserved segment with high outsourcing potential.
. Strategic states like California, Texas, and New York.
. Leverage operational cost advantages as compared to Market without compromising to deliver high-quality, affordable billing services.
Introduction :
The U.S. medical billing services market, valued at $5.7 billion in 2023, is projected to grow at a CAGR of 11.78%, reaching $12.26 billion by 2030 (Grand View Research). Key growth drivers include:
Increasing regulatory complexities, requiring outsourced billing solutions.
Adoption of cloud-based systems and AI-driven tools.
Rising trend of outsourcing by small to mid-sized practices to reduce costs and administrative burdens.
02
Introduction to an Ideal Billing Company
02
Introduction to an Ideal Billing Company
02
Introduction to an Ideal Billing Company
02
Introduction to an Ideal Billing Company
In today’s complex healthcare landscape, an ideal billing company serves as the backbone of financial stability and efficiency for medical practices. Such a company not only streamlines the revenue cycle but also ensures compliance, transparency, and adaptability to the evolving demands of the healthcare industry.
At its core, an ideal billing company offers end-to-end revenue cycle management (RCM) services, covering patient registration, claims submission, denial management, and account receivables follow-up. The company functions as a strategic partner, allowing healthcare providers to focus on patient care while ensuring their financial operations run seamlessly.
In today’s complex healthcare landscape, an ideal billing company serves as the backbone of financial stability and efficiency for medical practices. Such a company not only streamlines the revenue cycle but also ensures compliance, transparency, and adaptability to the evolving demands of the healthcare industry.
At its core, an ideal billing company offers end-to-end revenue cycle management (RCM) services, covering patient registration, claims submission, denial management, and account receivables follow-up. The company functions as a strategic partner, allowing healthcare providers to focus on patient care while ensuring their financial operations run seamlessly.
In today’s complex healthcare landscape, an ideal billing company serves as the backbone of financial stability and efficiency for medical practices. Such a company not only streamlines the revenue cycle but also ensures compliance, transparency, and adaptability to the evolving demands of the healthcare industry.
At its core, an ideal billing company offers end-to-end revenue cycle management (RCM) services, covering patient registration, claims submission, denial management, and account receivables follow-up. The company functions as a strategic partner, allowing healthcare providers to focus on patient care while ensuring their financial operations run seamlessly.
In today’s complex healthcare landscape, an ideal billing company serves as the backbone of financial stability and efficiency for medical practices. Such a company not only streamlines the revenue cycle but also ensures compliance, transparency, and adaptability to the evolving demands of the healthcare industry.
At its core, an ideal billing company offers end-to-end revenue cycle management (RCM) services, covering patient registration, claims submission, denial management, and account receivables follow-up. The company functions as a strategic partner, allowing healthcare providers to focus on patient care while ensuring their financial operations run seamlessly.
Key Attributes of an Ideal Billing Company:
Accuracy and Compliance:
The ideal billing company adheres to the latest regulations, including HIPAA, and keeps up with constantly changing payer requirements and coding standards (e.g., ICD-10, CPT). This minimizes claim rejections and denials, ensuring consistent revenue flow.
Technological Integration:
By leveraging advanced billing software, AI-driven analytics, and automated workflows, an ideal billing company ensures faster turnaround times and better accuracy in claims processing. Integration with EHR/EMR systems and patient portals enhances communication and transparency.
Customized Services:
Recognizing that each practice has unique needs, the ideal billing company offers tailored services, such as credentialing, coding audits, or AR follow-ups, ensuring maximum efficiency for specific specialties, including family medicine, dental care, or advanced aesthetics.
Proactive Denial Management:
Effective denial management processes, including root cause analysis and trend monitoring, help reduce errors, speed up collections, and address recurrent issues.
Data-Driven Decision Making:
Robust reporting and analytics help practices understand their financial health. An ideal billing company provides actionable insights into claim trends, payment patterns, and performance metrics to empower informed decision-making.
Exceptional Client Support:
A dedicated account manager and support team ensure seamless communication and swift resolution of any issues. The focus remains on building trust and long-term partnerships with clients.
Scalability and Adaptability:
The ideal billing company grows with its clients, scaling operations to handle higher claim volumes or expanding services to cover new specialties or locations.
Key Attributes of an Ideal Billing Company:
Accuracy and Compliance:
The ideal billing company adheres to the latest regulations, including HIPAA, and keeps up with constantly changing payer requirements and coding standards (e.g., ICD-10, CPT). This minimizes claim rejections and denials, ensuring consistent revenue flow.
Technological Integration:
By leveraging advanced billing software, AI-driven analytics, and automated workflows, an ideal billing company ensures faster turnaround times and better accuracy in claims processing. Integration with EHR/EMR systems and patient portals enhances communication and transparency.
Customized Services:
Recognizing that each practice has unique needs, the ideal billing company offers tailored services, such as credentialing, coding audits, or AR follow-ups, ensuring maximum efficiency for specific specialties, including family medicine, dental care, or advanced aesthetics.
Proactive Denial Management:
Effective denial management processes, including root cause analysis and trend monitoring, help reduce errors, speed up collections, and address recurrent issues.
Data-Driven Decision Making:
Robust reporting and analytics help practices understand their financial health. An ideal billing company provides actionable insights into claim trends, payment patterns, and performance metrics to empower informed decision-making.
Exceptional Client Support:
A dedicated account manager and support team ensure seamless communication and swift resolution of any issues. The focus remains on building trust and long-term partnerships with clients.
Scalability and Adaptability:
The ideal billing company grows with its clients, scaling operations to handle higher claim volumes or expanding services to cover new specialties or locations.
Key Attributes of an Ideal Billing Company:
Accuracy and Compliance:
The ideal billing company adheres to the latest regulations, including HIPAA, and keeps up with constantly changing payer requirements and coding standards (e.g., ICD-10, CPT). This minimizes claim rejections and denials, ensuring consistent revenue flow.
Technological Integration:
By leveraging advanced billing software, AI-driven analytics, and automated workflows, an ideal billing company ensures faster turnaround times and better accuracy in claims processing. Integration with EHR/EMR systems and patient portals enhances communication and transparency.
Customized Services:
Recognizing that each practice has unique needs, the ideal billing company offers tailored services, such as credentialing, coding audits, or AR follow-ups, ensuring maximum efficiency for specific specialties, including family medicine, dental care, or advanced aesthetics.
Proactive Denial Management:
Effective denial management processes, including root cause analysis and trend monitoring, help reduce errors, speed up collections, and address recurrent issues.
Data-Driven Decision Making:
Robust reporting and analytics help practices understand their financial health. An ideal billing company provides actionable insights into claim trends, payment patterns, and performance metrics to empower informed decision-making.
Exceptional Client Support:
A dedicated account manager and support team ensure seamless communication and swift resolution of any issues. The focus remains on building trust and long-term partnerships with clients.
Scalability and Adaptability:
The ideal billing company grows with its clients, scaling operations to handle higher claim volumes or expanding services to cover new specialties or locations.
Key Attributes of an Ideal Billing Company:
Accuracy and Compliance:
The ideal billing company adheres to the latest regulations, including HIPAA, and keeps up with constantly changing payer requirements and coding standards (e.g., ICD-10, CPT). This minimizes claim rejections and denials, ensuring consistent revenue flow.
Technological Integration:
By leveraging advanced billing software, AI-driven analytics, and automated workflows, an ideal billing company ensures faster turnaround times and better accuracy in claims processing. Integration with EHR/EMR systems and patient portals enhances communication and transparency.
Customized Services:
Recognizing that each practice has unique needs, the ideal billing company offers tailored services, such as credentialing, coding audits, or AR follow-ups, ensuring maximum efficiency for specific specialties, including family medicine, dental care, or advanced aesthetics.
Proactive Denial Management:
Effective denial management processes, including root cause analysis and trend monitoring, help reduce errors, speed up collections, and address recurrent issues.
Data-Driven Decision Making:
Robust reporting and analytics help practices understand their financial health. An ideal billing company provides actionable insights into claim trends, payment patterns, and performance metrics to empower informed decision-making.
Exceptional Client Support:
A dedicated account manager and support team ensure seamless communication and swift resolution of any issues. The focus remains on building trust and long-term partnerships with clients.
Scalability and Adaptability:
The ideal billing company grows with its clients, scaling operations to handle higher claim volumes or expanding services to cover new specialties or locations.
Benefits to Providers:
Increased revenue and reduced administrative burden.
Enhanced patient satisfaction through transparent billing processes.
Lower operational costs compared to in-house billing teams.
An ideal billing company, like My Health Aiyin embodies these qualities, blending expertise with cutting-edge technology to transform healthcare billing into a hassle-free experience. With a focus on accuracy, compliance, and customer-centric services, such companies empower healthcare providers to achieve financial growth while dedicating more time to patient care.
Benefits to Providers:
Increased revenue and reduced administrative burden.
Enhanced patient satisfaction through transparent billing processes.
Lower operational costs compared to in-house billing teams.
An ideal billing company, like My Health Aiyin embodies these qualities, blending expertise with cutting-edge technology to transform healthcare billing into a hassle-free experience. With a focus on accuracy, compliance, and customer-centric services, such companies empower healthcare providers to achieve financial growth while dedicating more time to patient care.
Benefits to Providers:
Increased revenue and reduced administrative burden.
Enhanced patient satisfaction through transparent billing processes.
Lower operational costs compared to in-house billing teams.
An ideal billing company, like My Health Aiyin embodies these qualities, blending expertise with cutting-edge technology to transform healthcare billing into a hassle-free experience. With a focus on accuracy, compliance, and customer-centric services, such companies empower healthcare providers to achieve financial growth while dedicating more time to patient care.
Benefits to Providers:
Increased revenue and reduced administrative burden.
Enhanced patient satisfaction through transparent billing processes.
Lower operational costs compared to in-house billing teams.
An ideal billing company, like My Health Aiyin embodies these qualities, blending expertise with cutting-edge technology to transform healthcare billing into a hassle-free experience. With a focus on accuracy, compliance, and customer-centric services, such companies empower healthcare providers to achieve financial growth while dedicating more time to patient care.
03
Organizational Structure, Workflow, and Strategic Goals
03
Organizational Structure, Workflow, and Strategic Goals
03
Organizational Structure, Workflow, and Strategic Goals
03
Organizational Structure, Workflow, and Strategic Goals
Organizational Structure
The organization is designed to ensure optimal efficiency and collaboration, with clearly defined roles across leadership, billing and coding, claims management, compliance, credentialing, IT, and customer support.
Organizational Structure
The organization is designed to ensure optimal efficiency and collaboration, with clearly defined roles across leadership, billing and coding, claims management, compliance, credentialing, IT, and customer support.
Organizational Structure
The organization is designed to ensure optimal efficiency and collaboration, with clearly defined roles across leadership, billing and coding, claims management, compliance, credentialing, IT, and customer support.
Organizational Structure
The organization is designed to ensure optimal efficiency and collaboration, with clearly defined roles across leadership, billing and coding, claims management, compliance, credentialing, IT, and customer support.
1.Leadership and Executive Roles
1.1 Chief Executive Officer (CEO) Role:
Leads the company’s strategic vision and ensures growth and profitability.
Responsibilities: Develop long-term corporate strategies. Cultivate relationships with clients, investors, and regulators. Evaluate the company’s financial and operational performance.
Skills: Leadership, innovation, communication, and financial acumen.
1.2 Chief Operating Officer (COO) Role:
Manages daily operations to ensure seamless execution across departments.
Responsibilities: Supervise operational workflows and resolve inter-departmental challenges. Monitor KPIs to ensure operational efficiency. Implement process improvements.
Skills: Process optimization, operational expertise, and leadership.
1.3 Chief Financial Officer (CFO) Role:
Oversees financial planning, budgeting, and compliance.
Responsibilities: Prepare financial forecasts and budget reports. Manage investments and financial risks. Ensure compliance with tax regulations and financial reporting standards.
Skills: Financial modeling, risk analysis, and strategic planning.
1.4 Chief Information Officer (CIO) Role:
Oversees the company’s IT strategy and ensures a secure and scalable infrastructure.
Responsibilities: Manage IT systems integration and updates. Implement data protection protocols to meet HIPAA compliance. Evaluate and integrate emerging technologies like AI and RPA (Robotic Process Automation).
Skills: Healthcare IT knowledge, cybersecurity, and digital transformation.
1.Leadership and Executive Roles
1.1 Chief Executive Officer (CEO) Role:
Leads the company’s strategic vision and ensures growth and profitability.
Responsibilities: Develop long-term corporate strategies. Cultivate relationships with clients, investors, and regulators. Evaluate the company’s financial and operational performance.
Skills: Leadership, innovation, communication, and financial acumen.
1.2 Chief Operating Officer (COO) Role:
Manages daily operations to ensure seamless execution across departments.
Responsibilities: Supervise operational workflows and resolve inter-departmental challenges. Monitor KPIs to ensure operational efficiency. Implement process improvements.
Skills: Process optimization, operational expertise, and leadership.
1.3 Chief Financial Officer (CFO) Role:
Oversees financial planning, budgeting, and compliance.
Responsibilities: Prepare financial forecasts and budget reports. Manage investments and financial risks. Ensure compliance with tax regulations and financial reporting standards.
Skills: Financial modeling, risk analysis, and strategic planning.
1.4 Chief Information Officer (CIO) Role:
Oversees the company’s IT strategy and ensures a secure and scalable infrastructure.
Responsibilities: Manage IT systems integration and updates. Implement data protection protocols to meet HIPAA compliance. Evaluate and integrate emerging technologies like AI and RPA (Robotic Process Automation).
Skills: Healthcare IT knowledge, cybersecurity, and digital transformation.
1.Leadership and Executive Roles
1.1 Chief Executive Officer (CEO) Role:
Leads the company’s strategic vision and ensures growth and profitability.
Responsibilities: Develop long-term corporate strategies. Cultivate relationships with clients, investors, and regulators. Evaluate the company’s financial and operational performance.
Skills: Leadership, innovation, communication, and financial acumen.
1.2 Chief Operating Officer (COO) Role:
Manages daily operations to ensure seamless execution across departments.
Responsibilities: Supervise operational workflows and resolve inter-departmental challenges. Monitor KPIs to ensure operational efficiency. Implement process improvements.
Skills: Process optimization, operational expertise, and leadership.
1.3 Chief Financial Officer (CFO) Role:
Oversees financial planning, budgeting, and compliance.
Responsibilities: Prepare financial forecasts and budget reports. Manage investments and financial risks. Ensure compliance with tax regulations and financial reporting standards.
Skills: Financial modeling, risk analysis, and strategic planning.
1.4 Chief Information Officer (CIO) Role:
Oversees the company’s IT strategy and ensures a secure and scalable infrastructure.
Responsibilities: Manage IT systems integration and updates. Implement data protection protocols to meet HIPAA compliance. Evaluate and integrate emerging technologies like AI and RPA (Robotic Process Automation).
Skills: Healthcare IT knowledge, cybersecurity, and digital transformation.
1.Leadership and Executive Roles
1.1 Chief Executive Officer (CEO) Role:
Leads the company’s strategic vision and ensures growth and profitability.
Responsibilities: Develop long-term corporate strategies. Cultivate relationships with clients, investors, and regulators. Evaluate the company’s financial and operational performance.
Skills: Leadership, innovation, communication, and financial acumen.
1.2 Chief Operating Officer (COO) Role:
Manages daily operations to ensure seamless execution across departments.
Responsibilities: Supervise operational workflows and resolve inter-departmental challenges. Monitor KPIs to ensure operational efficiency. Implement process improvements.
Skills: Process optimization, operational expertise, and leadership.
1.3 Chief Financial Officer (CFO) Role:
Oversees financial planning, budgeting, and compliance.
Responsibilities: Prepare financial forecasts and budget reports. Manage investments and financial risks. Ensure compliance with tax regulations and financial reporting standards.
Skills: Financial modeling, risk analysis, and strategic planning.
1.4 Chief Information Officer (CIO) Role:
Oversees the company’s IT strategy and ensures a secure and scalable infrastructure.
Responsibilities: Manage IT systems integration and updates. Implement data protection protocols to meet HIPAA compliance. Evaluate and integrate emerging technologies like AI and RPA (Robotic Process Automation).
Skills: Healthcare IT knowledge, cybersecurity, and digital transformation.
2.Billing and Coding Department
2.1 Billing Roles
Billing Manager Role: Oversees billing processes and ensures compliance with payer requirements.
Responsibilities: Manage billing team performance and training. Resolve escalated issues with payers. Analyze billing workflows and recommend improvements.
Medical Biller Role: Prepares, submits, and tracks insurance claims.
Responsibilities: Verify patient insurance eligibility. Follow up on unpaid or rejected claims. Maintain accurate records of billing activities.
Billing Specialist Role: Handles patient balances, insurance follow-ups, and claim submissions.
Responsibilities: Prepare and submit error-free claims. Work with patients on payment plans and resolve disputes. Ensure compliance with billing standards.
2.2 Coding Roles Coding Manager
Role: Supervises the coding team and ensures accurate coding practices.
Responsibilities: Conduct coding audits for compliance. Train coders on updates to ICD-10, CPT, and HCPCS codes. Collaborate with medical providers for accurate documentation.
Medical Coder Role: Assigns standardized medical codes for billing purposes.
Responsibilities: Review patient charts and physician notes. Assign appropriate diagnosis and procedure codes. Stay updated on payer-specific coding guidelines.
Coder Specialist Role: Focuses on advanced coding for complex procedures and regulatory compliance.
Responsibilities: Conduct in-depth reviews of coding for specialties like surgery and radiology. Support billing teams in resolving coding-related denials.
Charge Entry Specialist Role: Inputs charges based on services rendered.
Responsibilities: Review clinical documentation for accuracy.
Enter charges into the billing system. Identify and correct any errors before submission.
2.Billing and Coding Department
2.1 Billing Roles
Billing Manager Role: Oversees billing processes and ensures compliance with payer requirements.
Responsibilities: Manage billing team performance and training. Resolve escalated issues with payers. Analyze billing workflows and recommend improvements.
Medical Biller Role: Prepares, submits, and tracks insurance claims.
Responsibilities: Verify patient insurance eligibility. Follow up on unpaid or rejected claims. Maintain accurate records of billing activities.
Billing Specialist Role: Handles patient balances, insurance follow-ups, and claim submissions.
Responsibilities: Prepare and submit error-free claims. Work with patients on payment plans and resolve disputes. Ensure compliance with billing standards.
2.2 Coding Roles Coding Manager
Role: Supervises the coding team and ensures accurate coding practices.
Responsibilities: Conduct coding audits for compliance. Train coders on updates to ICD-10, CPT, and HCPCS codes. Collaborate with medical providers for accurate documentation.
Medical Coder Role: Assigns standardized medical codes for billing purposes.
Responsibilities: Review patient charts and physician notes. Assign appropriate diagnosis and procedure codes. Stay updated on payer-specific coding guidelines.
Coder Specialist Role: Focuses on advanced coding for complex procedures and regulatory compliance.
Responsibilities: Conduct in-depth reviews of coding for specialties like surgery and radiology. Support billing teams in resolving coding-related denials.
Charge Entry Specialist Role: Inputs charges based on services rendered.
Responsibilities: Review clinical documentation for accuracy.
Enter charges into the billing system. Identify and correct any errors before submission.
2.Billing and Coding Department
2.1 Billing Roles
Billing Manager Role: Oversees billing processes and ensures compliance with payer requirements.
Responsibilities: Manage billing team performance and training. Resolve escalated issues with payers. Analyze billing workflows and recommend improvements.
Medical Biller Role: Prepares, submits, and tracks insurance claims.
Responsibilities: Verify patient insurance eligibility. Follow up on unpaid or rejected claims. Maintain accurate records of billing activities.
Billing Specialist Role: Handles patient balances, insurance follow-ups, and claim submissions.
Responsibilities: Prepare and submit error-free claims. Work with patients on payment plans and resolve disputes. Ensure compliance with billing standards.
2.2 Coding Roles Coding Manager
Role: Supervises the coding team and ensures accurate coding practices.
Responsibilities: Conduct coding audits for compliance. Train coders on updates to ICD-10, CPT, and HCPCS codes. Collaborate with medical providers for accurate documentation.
Medical Coder Role: Assigns standardized medical codes for billing purposes.
Responsibilities: Review patient charts and physician notes. Assign appropriate diagnosis and procedure codes. Stay updated on payer-specific coding guidelines.
Coder Specialist Role: Focuses on advanced coding for complex procedures and regulatory compliance.
Responsibilities: Conduct in-depth reviews of coding for specialties like surgery and radiology. Support billing teams in resolving coding-related denials.
Charge Entry Specialist Role: Inputs charges based on services rendered.
Responsibilities: Review clinical documentation for accuracy.
Enter charges into the billing system. Identify and correct any errors before submission.
2.Billing and Coding Department
2.1 Billing Roles
Billing Manager Role: Oversees billing processes and ensures compliance with payer requirements.
Responsibilities: Manage billing team performance and training. Resolve escalated issues with payers. Analyze billing workflows and recommend improvements.
Medical Biller Role: Prepares, submits, and tracks insurance claims.
Responsibilities: Verify patient insurance eligibility. Follow up on unpaid or rejected claims. Maintain accurate records of billing activities.
Billing Specialist Role: Handles patient balances, insurance follow-ups, and claim submissions.
Responsibilities: Prepare and submit error-free claims. Work with patients on payment plans and resolve disputes. Ensure compliance with billing standards.
2.2 Coding Roles Coding Manager
Role: Supervises the coding team and ensures accurate coding practices.
Responsibilities: Conduct coding audits for compliance. Train coders on updates to ICD-10, CPT, and HCPCS codes. Collaborate with medical providers for accurate documentation.
Medical Coder Role: Assigns standardized medical codes for billing purposes.
Responsibilities: Review patient charts and physician notes. Assign appropriate diagnosis and procedure codes. Stay updated on payer-specific coding guidelines.
Coder Specialist Role: Focuses on advanced coding for complex procedures and regulatory compliance.
Responsibilities: Conduct in-depth reviews of coding for specialties like surgery and radiology. Support billing teams in resolving coding-related denials.
Charge Entry Specialist Role: Inputs charges based on services rendered.
Responsibilities: Review clinical documentation for accuracy.
Enter charges into the billing system. Identify and correct any errors before submission.
3.Claims and Payment Management
Claims Management
Claims Manager
Role: Ensures efficient processing, submission, and resolution of claims.
Responsibilities: Track claim submission cycles.
Resolve escalated claims issues.
Collaborate with the AR and denials teams.
Claims Processor
Role: Reviews, prepares, and submits claims to payers.
Responsibilities: Ensure claims meet payer guidelines.
Track claim statuses and follow up on pending ones.
Identify recurring issues for resolution.
Accounts Receivable (AR) Specialist
Role: Monitors and collects outstanding payments.
Responsibilities: Manage aged receivables.
Negotiate payment terms with patients and providers.
Identify trends in payment delays and address root causes.
Denials Management Specialist
Role: Investigates and resolves denied claims.
Responsibilities: Analyze denial reasons and prepare appeals.
Collaborate with coding and billing teams to resolve recurring issues.
Maintain denial resolution reports.
Payment Management
Payment Posting Specialist
Role: Posts payments to patient accounts and reconciles discrepancies.
Responsibilities:
Post insurance and patient payments.
Match payments to remittance advice and identify discrepancies.
Update patient accounts and generate payment reports.
3.Claims and Payment Management
Claims Management
Claims Manager
Role: Ensures efficient processing, submission, and resolution of claims.
Responsibilities: Track claim submission cycles.
Resolve escalated claims issues.
Collaborate with the AR and denials teams.
Claims Processor
Role: Reviews, prepares, and submits claims to payers.
Responsibilities: Ensure claims meet payer guidelines.
Track claim statuses and follow up on pending ones.
Identify recurring issues for resolution.
Accounts Receivable (AR) Specialist
Role: Monitors and collects outstanding payments.
Responsibilities: Manage aged receivables.
Negotiate payment terms with patients and providers.
Identify trends in payment delays and address root causes.
Denials Management Specialist
Role: Investigates and resolves denied claims.
Responsibilities: Analyze denial reasons and prepare appeals.
Collaborate with coding and billing teams to resolve recurring issues.
Maintain denial resolution reports.
Payment Management
Payment Posting Specialist
Role: Posts payments to patient accounts and reconciles discrepancies.
Responsibilities:
Post insurance and patient payments.
Match payments to remittance advice and identify discrepancies.
Update patient accounts and generate payment reports.
3.Claims and Payment Management
Claims Management
Claims Manager
Role: Ensures efficient processing, submission, and resolution of claims.
Responsibilities: Track claim submission cycles.
Resolve escalated claims issues.
Collaborate with the AR and denials teams.
Claims Processor
Role: Reviews, prepares, and submits claims to payers.
Responsibilities: Ensure claims meet payer guidelines.
Track claim statuses and follow up on pending ones.
Identify recurring issues for resolution.
Accounts Receivable (AR) Specialist
Role: Monitors and collects outstanding payments.
Responsibilities: Manage aged receivables.
Negotiate payment terms with patients and providers.
Identify trends in payment delays and address root causes.
Denials Management Specialist
Role: Investigates and resolves denied claims.
Responsibilities: Analyze denial reasons and prepare appeals.
Collaborate with coding and billing teams to resolve recurring issues.
Maintain denial resolution reports.
Payment Management
Payment Posting Specialist
Role: Posts payments to patient accounts and reconciles discrepancies.
Responsibilities:
Post insurance and patient payments.
Match payments to remittance advice and identify discrepancies.
Update patient accounts and generate payment reports.
3.Claims and Payment Management
Claims Management
Claims Manager
Role: Ensures efficient processing, submission, and resolution of claims.
Responsibilities: Track claim submission cycles.
Resolve escalated claims issues.
Collaborate with the AR and denials teams.
Claims Processor
Role: Reviews, prepares, and submits claims to payers.
Responsibilities: Ensure claims meet payer guidelines.
Track claim statuses and follow up on pending ones.
Identify recurring issues for resolution.
Accounts Receivable (AR) Specialist
Role: Monitors and collects outstanding payments.
Responsibilities: Manage aged receivables.
Negotiate payment terms with patients and providers.
Identify trends in payment delays and address root causes.
Denials Management Specialist
Role: Investigates and resolves denied claims.
Responsibilities: Analyze denial reasons and prepare appeals.
Collaborate with coding and billing teams to resolve recurring issues.
Maintain denial resolution reports.
Payment Management
Payment Posting Specialist
Role: Posts payments to patient accounts and reconciles discrepancies.
Responsibilities:
Post insurance and patient payments.
Match payments to remittance advice and identify discrepancies.
Update patient accounts and generate payment reports.
4.Compliance and Quality
Assurance Compliance Officer
Role: Ensures adherence to healthcare regulations and internal policies.
Responsibilities: Conduct regular compliance audits.
Develop and enforce policies to meet payer requirements.
Monitor HIPAA compliance across operations.
Audit Manager
Role: Manages internal audits for claims and billing accuracy.
Responsibilities: Identify discrepancies in submitted claims.
Provide training on audit findings.
Ensure audit standards are followed.
Quality Assurance Specialist
Role: Reviews claims and processes for compliance and quality improvement.
Responsibilities: Implement quality assurance workflows.
Perform detailed claim reviews before submission.
Identify and mitigate quality issues.
4.Compliance and Quality
Assurance Compliance Officer
Role: Ensures adherence to healthcare regulations and internal policies.
Responsibilities: Conduct regular compliance audits.
Develop and enforce policies to meet payer requirements.
Monitor HIPAA compliance across operations.
Audit Manager
Role: Manages internal audits for claims and billing accuracy.
Responsibilities: Identify discrepancies in submitted claims.
Provide training on audit findings.
Ensure audit standards are followed.
Quality Assurance Specialist
Role: Reviews claims and processes for compliance and quality improvement.
Responsibilities: Implement quality assurance workflows.
Perform detailed claim reviews before submission.
Identify and mitigate quality issues.
4.Compliance and Quality
Assurance Compliance Officer
Role: Ensures adherence to healthcare regulations and internal policies.
Responsibilities: Conduct regular compliance audits.
Develop and enforce policies to meet payer requirements.
Monitor HIPAA compliance across operations.
Audit Manager
Role: Manages internal audits for claims and billing accuracy.
Responsibilities: Identify discrepancies in submitted claims.
Provide training on audit findings.
Ensure audit standards are followed.
Quality Assurance Specialist
Role: Reviews claims and processes for compliance and quality improvement.
Responsibilities: Implement quality assurance workflows.
Perform detailed claim reviews before submission.
Identify and mitigate quality issues.
4.Compliance and Quality
Assurance Compliance Officer
Role: Ensures adherence to healthcare regulations and internal policies.
Responsibilities: Conduct regular compliance audits.
Develop and enforce policies to meet payer requirements.
Monitor HIPAA compliance across operations.
Audit Manager
Role: Manages internal audits for claims and billing accuracy.
Responsibilities: Identify discrepancies in submitted claims.
Provide training on audit findings.
Ensure audit standards are followed.
Quality Assurance Specialist
Role: Reviews claims and processes for compliance and quality improvement.
Responsibilities: Implement quality assurance workflows.
Perform detailed claim reviews before submission.
Identify and mitigate quality issues.
5.Credentialing
Credentialing Manager
Role: Oversees the credentialing and enrollment process for providers.
Responsibilities: Manage provider re-credentialing schedules.
Ensure credentialing compliance with payers.
Maintain a database of credentialing records.
Credentialing Specialist
Role: Verifies and processes Provider credentialing applications.
Responsibilities: Collect and validate provider documents.
Submit applications to insurance networks.
Track credentialing application statuses.
Provider Enrollment Specialist
Role: Manages provider enrollments with insurance payers.
Responsibilities: Complete enrollment applications accurately.
Communicate with payers on provider statuses. Monitor re-enrollment timelines.
5.Credentialing
Credentialing Manager
Role: Oversees the credentialing and enrollment process for providers.
Responsibilities: Manage provider re-credentialing schedules.
Ensure credentialing compliance with payers.
Maintain a database of credentialing records.
Credentialing Specialist
Role: Verifies and processes Provider credentialing applications.
Responsibilities: Collect and validate provider documents.
Submit applications to insurance networks.
Track credentialing application statuses.
Provider Enrollment Specialist
Role: Manages provider enrollments with insurance payers.
Responsibilities: Complete enrollment applications accurately.
Communicate with payers on provider statuses. Monitor re-enrollment timelines.
5.Credentialing
Credentialing Manager
Role: Oversees the credentialing and enrollment process for providers.
Responsibilities: Manage provider re-credentialing schedules.
Ensure credentialing compliance with payers.
Maintain a database of credentialing records.
Credentialing Specialist
Role: Verifies and processes Provider credentialing applications.
Responsibilities: Collect and validate provider documents.
Submit applications to insurance networks.
Track credentialing application statuses.
Provider Enrollment Specialist
Role: Manages provider enrollments with insurance payers.
Responsibilities: Complete enrollment applications accurately.
Communicate with payers on provider statuses. Monitor re-enrollment timelines.
5.Credentialing
Credentialing Manager
Role: Oversees the credentialing and enrollment process for providers.
Responsibilities: Manage provider re-credentialing schedules.
Ensure credentialing compliance with payers.
Maintain a database of credentialing records.
Credentialing Specialist
Role: Verifies and processes Provider credentialing applications.
Responsibilities: Collect and validate provider documents.
Submit applications to insurance networks.
Track credentialing application statuses.
Provider Enrollment Specialist
Role: Manages provider enrollments with insurance payers.
Responsibilities: Complete enrollment applications accurately.
Communicate with payers on provider statuses. Monitor re-enrollment timelines.
6.IT and Cybersecurity
Cybersecurity Manager
Role: Protects sensitive patient data from cyber threats.
Responsibilities: Implement firewalls and security protocols.
Conduct regular vulnerability assessments.
Respond to cybersecurity incidents.
Information Security Officer
Role: Ensures compliance with HIPAA and data protection laws.
Responsibilities: Develop and maintain IT security policies.
Conduct risk assessments and audits.
Train staff on data security protocols.
IT Manager
Role: Manages the IT infrastructure and system integrations.
Responsibilities: Maintain billing software and system uptime.
Support staff with IT issues. Implement RPA for automation.
6.IT and Cybersecurity
Cybersecurity Manager
Role: Protects sensitive patient data from cyber threats.
Responsibilities: Implement firewalls and security protocols.
Conduct regular vulnerability assessments.
Respond to cybersecurity incidents.
Information Security Officer
Role: Ensures compliance with HIPAA and data protection laws.
Responsibilities: Develop and maintain IT security policies.
Conduct risk assessments and audits.
Train staff on data security protocols.
IT Manager
Role: Manages the IT infrastructure and system integrations.
Responsibilities: Maintain billing software and system uptime.
Support staff with IT issues. Implement RPA for automation.
6.IT and Cybersecurity
Cybersecurity Manager
Role: Protects sensitive patient data from cyber threats.
Responsibilities: Implement firewalls and security protocols.
Conduct regular vulnerability assessments.
Respond to cybersecurity incidents.
Information Security Officer
Role: Ensures compliance with HIPAA and data protection laws.
Responsibilities: Develop and maintain IT security policies.
Conduct risk assessments and audits.
Train staff on data security protocols.
IT Manager
Role: Manages the IT infrastructure and system integrations.
Responsibilities: Maintain billing software and system uptime.
Support staff with IT issues. Implement RPA for automation.
6.IT and Cybersecurity
Cybersecurity Manager
Role: Protects sensitive patient data from cyber threats.
Responsibilities: Implement firewalls and security protocols.
Conduct regular vulnerability assessments.
Respond to cybersecurity incidents.
Information Security Officer
Role: Ensures compliance with HIPAA and data protection laws.
Responsibilities: Develop and maintain IT security policies.
Conduct risk assessments and audits.
Train staff on data security protocols.
IT Manager
Role: Manages the IT infrastructure and system integrations.
Responsibilities: Maintain billing software and system uptime.
Support staff with IT issues. Implement RPA for automation.
7.Customer Support
Client Relationship Manager
Role: Builds long-term relationships with clients.
Responsibilities: Provide regular status updates on claim performance.
Address client concerns and escalate issues as needed.
Customer Service Representative
Role: Assists patients and providers with inquiries.
Responsibilities: Handle calls regarding billing or payment issues.
Resolve disputes with professionalism.
Patient Account Representative
Role: Helps patients understand billing and payment options.
Responsibilities: Set up payment plans for patients.
Explain insurance policies and out-of-pocket expenses.
Strategic Goals
Goal 1: Operational Excellence
Objective: Reduce average claim submission time by 25%.
KPI: Claim processing cycle time.
Goal 2: Enhanced Compliance
Objective: Achieve zero compliance breaches.
KPI: Number of audits passed without discrepancies.
Goal 3: Client Satisfaction
Objective: Maintain a client retention rate of 98%.
KPI: Net promoter score (NPS).
Goal 4: Financial Growth
Objective: Increase revenue by 30% within 12 months.
KPI: Monthly revenue growth rate.
7.Customer Support
Client Relationship Manager
Role: Builds long-term relationships with clients.
Responsibilities: Provide regular status updates on claim performance.
Address client concerns and escalate issues as needed.
Customer Service Representative
Role: Assists patients and providers with inquiries.
Responsibilities: Handle calls regarding billing or payment issues.
Resolve disputes with professionalism.
Patient Account Representative
Role: Helps patients understand billing and payment options.
Responsibilities: Set up payment plans for patients.
Explain insurance policies and out-of-pocket expenses.
Strategic Goals
Goal 1: Operational Excellence
Objective: Reduce average claim submission time by 25%.
KPI: Claim processing cycle time.
Goal 2: Enhanced Compliance
Objective: Achieve zero compliance breaches.
KPI: Number of audits passed without discrepancies.
Goal 3: Client Satisfaction
Objective: Maintain a client retention rate of 98%.
KPI: Net promoter score (NPS).
Goal 4: Financial Growth
Objective: Increase revenue by 30% within 12 months.
KPI: Monthly revenue growth rate.
7.Customer Support
Client Relationship Manager
Role: Builds long-term relationships with clients.
Responsibilities: Provide regular status updates on claim performance.
Address client concerns and escalate issues as needed.
Customer Service Representative
Role: Assists patients and providers with inquiries.
Responsibilities: Handle calls regarding billing or payment issues.
Resolve disputes with professionalism.
Patient Account Representative
Role: Helps patients understand billing and payment options.
Responsibilities: Set up payment plans for patients.
Explain insurance policies and out-of-pocket expenses.
Strategic Goals
Goal 1: Operational Excellence
Objective: Reduce average claim submission time by 25%.
KPI: Claim processing cycle time.
Goal 2: Enhanced Compliance
Objective: Achieve zero compliance breaches.
KPI: Number of audits passed without discrepancies.
Goal 3: Client Satisfaction
Objective: Maintain a client retention rate of 98%.
KPI: Net promoter score (NPS).
Goal 4: Financial Growth
Objective: Increase revenue by 30% within 12 months.
KPI: Monthly revenue growth rate.
7.Customer Support
Client Relationship Manager
Role: Builds long-term relationships with clients.
Responsibilities: Provide regular status updates on claim performance.
Address client concerns and escalate issues as needed.
Customer Service Representative
Role: Assists patients and providers with inquiries.
Responsibilities: Handle calls regarding billing or payment issues.
Resolve disputes with professionalism.
Patient Account Representative
Role: Helps patients understand billing and payment options.
Responsibilities: Set up payment plans for patients.
Explain insurance policies and out-of-pocket expenses.
Strategic Goals
Goal 1: Operational Excellence
Objective: Reduce average claim submission time by 25%.
KPI: Claim processing cycle time.
Goal 2: Enhanced Compliance
Objective: Achieve zero compliance breaches.
KPI: Number of audits passed without discrepancies.
Goal 3: Client Satisfaction
Objective: Maintain a client retention rate of 98%.
KPI: Net promoter score (NPS).
Goal 4: Financial Growth
Objective: Increase revenue by 30% within 12 months.
KPI: Monthly revenue growth rate.
04
Core Services
04
Core Services
04
Core Services
04
Core Services


We verify insurance coverage and confirm patient eligibility to ensure all authorizations are in place before services are provided, minimizing delays and denials.
Verification & Prior Authorization Services
We verify insurance coverage and confirm patient eligibility to ensure all authorizations are in place before services are provided, minimizing delays and denials.
Verification & Prior Authorization Services
Tap to flip
We verify insurance coverage and confirm patient eligibility to ensure all authorizations are in place before services are provided, minimizing delays and denials.
Verification & Prior Authorization Services
Tap to flip
We verify insurance coverage and confirm patient eligibility to ensure all authorizations are in place before services are provided, minimizing delays and denials.
Verification & Prior Authorization Services
Tap to flip
Our comprehensive RCM services manage the entire financial cycle, from charge capture to collections, enhancing operational efficiency and increasing revenue while reducing costs.
Revenue Cycle Management (RCM) Services
Our comprehensive RCM services manage the entire financial cycle, from charge capture to collections, enhancing operational efficiency and increasing revenue while reducing costs.
Revenue Cycle Management (RCM) Services
Tap to flip
Our comprehensive RCM services manage the entire financial cycle, from charge capture to collections, enhancing operational efficiency and increasing revenue while reducing costs.
Revenue Cycle Management (RCM) Services
Tap to flip
Our comprehensive RCM services manage the entire financial cycle, from charge capture to collections, enhancing operational efficiency and increasing revenue while reducing costs.
Revenue Cycle Management (RCM) Services
Tap to flip
We streamline credentialing, ensuring that all qualifications, licenses, and certifications are up to date, facilitating accurate and timely reimbursements.
Physician Credentialing Services
We streamline credentialing, ensuring that all qualifications, licenses, and certifications are up to date, facilitating accurate and timely reimbursements.
Physician Credentialing Services
Tap to flip
We streamline credentialing, ensuring that all qualifications, licenses, and certifications are up to date, facilitating accurate and timely reimbursements.
Physician Credentialing Services
Tap to flip
We streamline credentialing, ensuring that all qualifications, licenses, and certifications are up to date, facilitating accurate and timely reimbursements.
Physician Credentialing Services
Tap to flip
With advanced expertise, we ensure high claim acceptance rates, compliance with regulations, and reduce claim denials, maximizing reimbursement and minimizing errors.
Medical Billing & Coding Services
With advanced expertise, we ensure high claim acceptance rates, compliance with regulations, and reduce claim denials, maximizing reimbursement and minimizing errors.
Medical Billing & Coding Services
Tap to flip
With advanced expertise, we ensure high claim acceptance rates, compliance with regulations, and reduce claim denials, maximizing reimbursement and minimizing errors.
Medical Billing & Coding Services
Tap to flip
With advanced expertise, we ensure high claim acceptance rates, compliance with regulations, and reduce claim denials, maximizing reimbursement and minimizing errors.
Medical Billing & Coding Services
Tap to flip
Our tailored billing solutions for ambulatory surgical centers reduce administrative burdens, improve operational efficiency, and ensure timely reimbursement.
Ambulatory Surgical Center Billing
Our tailored billing solutions for ambulatory surgical centers reduce administrative burdens, improve operational efficiency, and ensure timely reimbursement.
Ambulatory Surgical Center Billing
Tap to flip
Our tailored billing solutions for ambulatory surgical centers reduce administrative burdens, improve operational efficiency, and ensure timely reimbursement.
Ambulatory Surgical Center Billing
Tap to flip
Our tailored billing solutions for ambulatory surgical centers reduce administrative burdens, improve operational efficiency, and ensure timely reimbursement.
Ambulatory Surgical Center Billing
Tap to flip
Rigorous audits uncover operational inefficiencies, errors, and compliance gaps, helping to improve billing accuracy, reduce risks, and optimize revenue.
Billing & Coding Audit Service
Rigorous audits uncover operational inefficiencies, errors, and compliance gaps, helping to improve billing accuracy, reduce risks, and optimize revenue.
Billing & Coding Audit Service
Tap to flip
Rigorous audits uncover operational inefficiencies, errors, and compliance gaps, helping to improve billing accuracy, reduce risks, and optimize revenue.
Billing & Coding Audit Service
Tap to flip
Rigorous audits uncover operational inefficiencies, errors, and compliance gaps, helping to improve billing accuracy, reduce risks, and optimize revenue.
Billing & Coding Audit Service
Tap to flip
We manage patient appointments, streamline scheduling, and enhance patient satisfaction, improving overall practice efficiency and patient flow.
Contact Center & Patient Scheduling Services
We manage patient appointments, streamline scheduling, and enhance patient satisfaction, improving overall practice efficiency and patient flow.
Contact Center & Patient Scheduling Services
Tap to flip
We manage patient appointments, streamline scheduling, and enhance patient satisfaction, improving overall practice efficiency and patient flow.
Contact Center & Patient Scheduling Services
Tap to flip
We manage patient appointments, streamline scheduling, and enhance patient satisfaction, improving overall practice efficiency and patient flow.
Contact Center & Patient Scheduling Services
Tap to flip
Our proactive strategies address accounts receivable and denials, reducing outstanding balances and ensuring timely reimbursements, improving cash flow.
AR & Denial Management Services
Our proactive strategies address accounts receivable and denials, reducing outstanding balances and ensuring timely reimbursements, improving cash flow.
AR & Denial Management Services
Tap to flip
Our proactive strategies address accounts receivable and denials, reducing outstanding balances and ensuring timely reimbursements, improving cash flow.
AR & Denial Management Services
Tap to flip
Our proactive strategies address accounts receivable and denials, reducing outstanding balances and ensuring timely reimbursements, improving cash flow.
AR & Denial Management Services
Tap to flip
We recover outstanding balances efficiently and respectfully, improving your practice's cash flow while maintaining positive patient relationships.
Patient Collections Services
We recover outstanding balances efficiently and respectfully, improving your practice's cash flow while maintaining positive patient relationships.
Patient Collections Services
Tap to flip
We recover outstanding balances efficiently and respectfully, improving your practice's cash flow while maintaining positive patient relationships.
Patient Collections Services
Tap to flip
We recover outstanding balances efficiently and respectfully, improving your practice's cash flow while maintaining positive patient relationships.
Patient Collections Services
Tap to flip
We ensure that your practice remains compliant with healthcare regulations, including HIPAA and insurance requirements, safeguarding your practice against penalties.
Compliance & Regulatory Services
We ensure that your practice remains compliant with healthcare regulations, including HIPAA and insurance requirements, safeguarding your practice against penalties.
Compliance & Regulatory Services
Tap to flip
We ensure that your practice remains compliant with healthcare regulations, including HIPAA and insurance requirements, safeguarding your practice against penalties.
Compliance & Regulatory Services
Tap to flip
We ensure that your practice remains compliant with healthcare regulations, including HIPAA and insurance requirements, safeguarding your practice against penalties.
Compliance & Regulatory Services
Tap to flip
We handle the submission, follow-up, and resolution of insurance claims, ensuring that claims are processed accurately and efficiently, reducing the chances of rejections or delays.
Insurance Claims Management
We handle the submission, follow-up, and resolution of insurance claims, ensuring that claims are processed accurately and efficiently, reducing the chances of rejections or delays.
Insurance Claims Management
Tap to flip
We handle the submission, follow-up, and resolution of insurance claims, ensuring that claims are processed accurately and efficiently, reducing the chances of rejections or delays.
Insurance Claims Management
Tap to flip
We handle the submission, follow-up, and resolution of insurance claims, ensuring that claims are processed accurately and efficiently, reducing the chances of rejections or delays.
Insurance Claims Management
Tap to flip
We ensure that medical coding follows the latest industry standards, maintaining compliance with payer requirements, and reducing the risk of audits or penalties.
Medical Coding Compliance Services
We ensure that medical coding follows the latest industry standards, maintaining compliance with payer requirements, and reducing the risk of audits or penalties.
Medical Coding Compliance Services
Tap to flip
We ensure that medical coding follows the latest industry standards, maintaining compliance with payer requirements, and reducing the risk of audits or penalties.
Medical Coding Compliance Services
Tap to flip
We ensure that medical coding follows the latest industry standards, maintaining compliance with payer requirements, and reducing the risk of audits or penalties.
Medical Coding Compliance Services
Tap to flip
05
Target Specialities
05
Target Specialities
05
Target Specialities
05
Target Specialities


We streamline billing for comprehensive care, covering preventive services and chronic condition management for all age groups
Family Practice & Primary Care
We streamline billing for comprehensive care, covering preventive services and chronic condition management for all age groups
Family Practice & Primary Care
Tap to flip
We streamline billing for comprehensive care, covering preventive services and chronic condition management for all age groups
Family Practice & Primary Care
Tap to flip
We streamline billing for comprehensive care, covering preventive services and chronic condition management for all age groups
Family Practice & Primary Care
Tap to flip
Our billing expertise ensures accurate claims for elderly care, addressing chronic conditions and specialized long-term treatments
Geriatrics
Our billing expertise ensures accurate claims for elderly care, addressing chronic conditions and specialized long-term treatments
Geriatrics
Tap to flip
Our billing expertise ensures accurate claims for elderly care, addressing chronic conditions and specialized long-term treatments
Geriatrics
Tap to flip
Our billing expertise ensures accurate claims for elderly care, addressing chronic conditions and specialized long-term treatments
Geriatrics
Tap to flip
We provide tailored billing for child-focused care, including vaccinations, developmental assessments, and chronic condition management
Pediatrics
We provide tailored billing for child-focused care, including vaccinations, developmental assessments, and chronic condition management
Pediatrics
Tap to flip
We provide tailored billing for child-focused care, including vaccinations, developmental assessments, and chronic condition management
Pediatrics
Tap to flip
We provide tailored billing for child-focused care, including vaccinations, developmental assessments, and chronic condition management
Pediatrics
Tap to flip
Accurate claims processing for diagnostics, specialized therapies, and treatment plans with full regulatory compliance
Infectious Diseases
Accurate claims processing for diagnostics, specialized therapies, and treatment plans with full regulatory compliance
Infectious Diseases
Tap to flip
Accurate claims processing for diagnostics, specialized therapies, and treatment plans with full regulatory compliance
Infectious Diseases
Tap to flip
Accurate claims processing for diagnostics, specialized therapies, and treatment plans with full regulatory compliance
Infectious Diseases
Tap to flip
We manage complex billing for chronic diseases, preventive care, and adult patient-focused services to optimize revenue cycles
Internal Medicine
We manage complex billing for chronic diseases, preventive care, and adult patient-focused services to optimize revenue cycles
Internal Medicine
Tap to flip
We manage complex billing for chronic diseases, preventive care, and adult patient-focused services to optimize revenue cycles
Internal Medicine
Tap to flip
We manage complex billing for chronic diseases, preventive care, and adult patient-focused services to optimize revenue cycles
Internal Medicine
Tap to flip
Our solutions ensure precise billing for diagnostics, procedures, and treatments, supporting comprehensive cardiac care
Cardiology
Our solutions ensure precise billing for diagnostics, procedures, and treatments, supporting comprehensive cardiac care
Cardiology
Tap to flip
Our solutions ensure precise billing for diagnostics, procedures, and treatments, supporting comprehensive cardiac care
Cardiology
Tap to flip
Our solutions ensure precise billing for diagnostics, procedures, and treatments, supporting comprehensive cardiac care
Cardiology
Tap to flip
Seamless claims processing for joint replacements, sports injuries, and physical therapy services to reduce administrative burdens.
Orthopedic Surgery
Seamless claims processing for joint replacements, sports injuries, and physical therapy services to reduce administrative burdens.
Orthopedic Surgery
Tap to flip
Seamless claims processing for joint replacements, sports injuries, and physical therapy services to reduce administrative burdens.
Orthopedic Surgery
Tap to flip
Seamless claims processing for joint replacements, sports injuries, and physical therapy services to reduce administrative burdens.
Orthopedic Surgery
Tap to flip
Efficient billing management for inpatient and outpatient procedures, ensuring compliance and timely reimbursements
General Surgery
Efficient billing management for inpatient and outpatient procedures, ensuring compliance and timely reimbursements
General Surgery
Tap to flip
Efficient billing management for inpatient and outpatient procedures, ensuring compliance and timely reimbursements
General Surgery
Tap to flip
Efficient billing management for inpatient and outpatient procedures, ensuring compliance and timely reimbursements
General Surgery
Tap to flip
Our expertise covers anesthesia billing for surgical, procedural, and pain management services with accuracy and compliance
Anesthesiology
Our expertise covers anesthesia billing for surgical, procedural, and pain management services with accuracy and compliance
Anesthesiology
Tap to flip
Our expertise covers anesthesia billing for surgical, procedural, and pain management services with accuracy and compliance
Anesthesiology
Tap to flip
Our expertise covers anesthesia billing for surgical, procedural, and pain management services with accuracy and compliance
Anesthesiology
Tap to flip
06
Tools and Technologies
06
Tools and Technologies
06
Tools and Technologies
06
Tools and Technologies


Customizable and affordable, Practice EHR streamlines medical billing and enhances practice efficiency, tailored to meet the unique needs of healthcare providers.
Practice EHR
Customizable and affordable, Practice EHR streamlines medical billing and enhances practice efficiency, tailored to meet the unique needs of healthcare providers.
Practice EHR
Tap to flip
Customizable and affordable, Practice EHR streamlines medical billing and enhances practice efficiency, tailored to meet the unique needs of healthcare providers.
Practice EHR
Tap to flip
Customizable and affordable, Practice EHR streamlines medical billing and enhances practice efficiency, tailored to meet the unique needs of healthcare providers.
Practice EHR
Tap to flip
Tebra provides a holistic system with a dedicated success coach, offering seamless functionality across multiple platforms to optimize practice management.
Tebra
Tebra provides a holistic system with a dedicated success coach, offering seamless functionality across multiple platforms to optimize practice management.
Tebra
Tap to flip
Tebra provides a holistic system with a dedicated success coach, offering seamless functionality across multiple platforms to optimize practice management.
Tebra
Tap to flip
Tebra provides a holistic system with a dedicated success coach, offering seamless functionality across multiple platforms to optimize practice management.
Tebra
Tap to flip
Office Ally offers user-friendly, scalable solutions for medical billing, EHR, and clearinghouse services, designed to support practices of all sizes.
Office Ally
Office Ally offers user-friendly, scalable solutions for medical billing, EHR, and clearinghouse services, designed to support practices of all sizes.
Office Ally
Tap to flip
Office Ally offers user-friendly, scalable solutions for medical billing, EHR, and clearinghouse services, designed to support practices of all sizes.
Office Ally
Tap to flip
Office Ally offers user-friendly, scalable solutions for medical billing, EHR, and clearinghouse services, designed to support practices of all sizes.
Office Ally
Tap to flip
eClinicalWorks integrates EMR, mobile access, and a patient portal, streamlining both clinical and billing workflows for healthcare providers.
eClinicalWorks
eClinicalWorks integrates EMR, mobile access, and a patient portal, streamlining both clinical and billing workflows for healthcare providers.
eClinicalWorks
Tap to flip
eClinicalWorks integrates EMR, mobile access, and a patient portal, streamlining both clinical and billing workflows for healthcare providers.
eClinicalWorks
Tap to flip
eClinicalWorks integrates EMR, mobile access, and a patient portal, streamlining both clinical and billing workflows for healthcare providers.
eClinicalWorks
Tap to flip
AdvancedMD delivers an integrated platform for billing, practice management, and EHR, optimizing revenue cycles and financial operations for various specialties.
AdvancedMD
AdvancedMD delivers an integrated platform for billing, practice management, and EHR, optimizing revenue cycles and financial operations for various specialties.
AdvancedMD
Tap to flip
AdvancedMD delivers an integrated platform for billing, practice management, and EHR, optimizing revenue cycles and financial operations for various specialties.
AdvancedMD
Tap to flip
AdvancedMD delivers an integrated platform for billing, practice management, and EHR, optimizing revenue cycles and financial operations for various specialties.
AdvancedMD
Tap to flip
Athenahealth offers comprehensive EHR solutions, enhancing clinical workflows and billing accuracy through a cloud-based platform that benefits both administrative and clinical processes.
Athenahealth
Athenahealth offers comprehensive EHR solutions, enhancing clinical workflows and billing accuracy through a cloud-based platform that benefits both administrative and clinical processes.
Athenahealth
Tap to flip
Athenahealth offers comprehensive EHR solutions, enhancing clinical workflows and billing accuracy through a cloud-based platform that benefits both administrative and clinical processes.
Athenahealth
Tap to flip
Athenahealth offers comprehensive EHR solutions, enhancing clinical workflows and billing accuracy through a cloud-based platform that benefits both administrative and clinical processes.
Athenahealth
Tap to flip
Practice Fusion provides a broad range of EHR functionalities, offering an intuitive interface that integrates seamlessly with billing and scheduling systems.
Practice Fusion
Practice Fusion provides a broad range of EHR functionalities, offering an intuitive interface that integrates seamlessly with billing and scheduling systems.
Practice Fusion
Tap to flip
Practice Fusion provides a broad range of EHR functionalities, offering an intuitive interface that integrates seamlessly with billing and scheduling systems.
Practice Fusion
Tap to flip
Practice Fusion provides a broad range of EHR functionalities, offering an intuitive interface that integrates seamlessly with billing and scheduling systems.
Practice Fusion
Tap to flip
Align Software supports strategic practice growth management with a user-friendly interface, enhancing billing and clinical workflows for growing practices.
Align Software
Align Software supports strategic practice growth management with a user-friendly interface, enhancing billing and clinical workflows for growing practices.
Align Software
Tap to flip
Align Software supports strategic practice growth management with a user-friendly interface, enhancing billing and clinical workflows for growing practices.
Align Software
Tap to flip
Align Software supports strategic practice growth management with a user-friendly interface, enhancing billing and clinical workflows for growing practices.
Align Software
Tap to flip
ChiroSpring specializes in chiropractic billing and EHR solutions, offering flexible pricing tiers to suit practices of different sizes.
ChiroSpring
ChiroSpring specializes in chiropractic billing and EHR solutions, offering flexible pricing tiers to suit practices of different sizes.
ChiroSpring
Tap to flip
ChiroSpring specializes in chiropractic billing and EHR solutions, offering flexible pricing tiers to suit practices of different sizes.
ChiroSpring
Tap to flip
ChiroSpring specializes in chiropractic billing and EHR solutions, offering flexible pricing tiers to suit practices of different sizes.
ChiroSpring
Tap to flip
Availity offers a comprehensive health information network and cost-effective clearinghouse solutions to improve claims processing efficiency.
Availity
Availity offers a comprehensive health information network and cost-effective clearinghouse solutions to improve claims processing efficiency.
Availity
Tap to flip
Availity offers a comprehensive health information network and cost-effective clearinghouse solutions to improve claims processing efficiency.
Availity
Tap to flip
Availity offers a comprehensive health information network and cost-effective clearinghouse solutions to improve claims processing efficiency.
Availity
Tap to flip
CareCloud is a cloud-based platform integrating medical billing, practice management, and EHR features to streamline workflows and boost practice revenue.
CareCloud
CareCloud is a cloud-based platform integrating medical billing, practice management, and EHR features to streamline workflows and boost practice revenue.
CareCloud
Tap to flip
CareCloud is a cloud-based platform integrating medical billing, practice management, and EHR features to streamline workflows and boost practice revenue.
CareCloud
Tap to flip
CareCloud is a cloud-based platform integrating medical billing, practice management, and EHR features to streamline workflows and boost practice revenue.
CareCloud
Tap to flip
NextGen Healthcare combines billing, EHR, and practice management tools to optimize revenue cycles and enhance financial management for healthcare providers.
NextGen Healthcare
NextGen Healthcare combines billing, EHR, and practice management tools to optimize revenue cycles and enhance financial management for healthcare providers.
NextGen Healthcare
Tap to flip
NextGen Healthcare combines billing, EHR, and practice management tools to optimize revenue cycles and enhance financial management for healthcare providers.
NextGen Healthcare
Tap to flip
NextGen Healthcare combines billing, EHR, and practice management tools to optimize revenue cycles and enhance financial management for healthcare providers.
NextGen Healthcare
Tap to flip
DrChrono offers customizable billing, EHR, and practice management tools, known for its user-friendly interface and cloud-based accessibility to improve practice efficiency
DrChrono
DrChrono offers customizable billing, EHR, and practice management tools, known for its user-friendly interface and cloud-based accessibility to improve practice efficiency
DrChrono
Tap to flip
DrChrono offers customizable billing, EHR, and practice management tools, known for its user-friendly interface and cloud-based accessibility to improve practice efficiency
DrChrono
Tap to flip
DrChrono offers customizable billing, EHR, and practice management tools, known for its user-friendly interface and cloud-based accessibility to improve practice efficiency
DrChrono
Tap to flip
07
Revenue Cycle Lifecycle
07
Revenue Cycle Lifecycle
07
Revenue Cycle Lifecycle
07
Revenue Cycle Lifecycle
1. Credentialing
Purpose: Establish and maintain healthcare providers’ eligibility to deliver services within insurance networks.
Verification of Credentials: Validate provider education, certifications, licensure, and professional history.
Enrollment with Payers: Submit and track applications for providers to join insurance networks.
Compliance Assurance: Ensure providers meet state and federal regulatory requirements.
Re-Credentialing: Manage periodic re-verification processes to maintain payer participation.
1. Credentialing
Purpose: Establish and maintain healthcare providers’ eligibility to deliver services within insurance networks.
Verification of Credentials: Validate provider education, certifications, licensure, and professional history.
Enrollment with Payers: Submit and track applications for providers to join insurance networks.
Compliance Assurance: Ensure providers meet state and federal regulatory requirements.
Re-Credentialing: Manage periodic re-verification processes to maintain payer participation.
1. Credentialing
Purpose: Establish and maintain healthcare providers’ eligibility to deliver services within insurance networks.
Verification of Credentials: Validate provider education, certifications, licensure, and professional history.
Enrollment with Payers: Submit and track applications for providers to join insurance networks.
Compliance Assurance: Ensure providers meet state and federal regulatory requirements.
Re-Credentialing: Manage periodic re-verification processes to maintain payer participation.
1. Credentialing
Purpose: Establish and maintain healthcare providers’ eligibility to deliver services within insurance networks.
Verification of Credentials: Validate provider education, certifications, licensure, and professional history.
Enrollment with Payers: Submit and track applications for providers to join insurance networks.
Compliance Assurance: Ensure providers meet state and federal regulatory requirements.
Re-Credentialing: Manage periodic re-verification processes to maintain payer participation.
08
Common Challenges in Medical Billing.
08
Common Challenges in Medical Billing.
08
Common Challenges in Medical Billing.
08
Common Challenges in Medical Billing.
Claim denials and rejections: Due to incorrect coding or missing information.
Patient financial responsibility confusion: Lack of clarity about their share of the cost.
AR delays: Long payment cycles causing cash flow issues.
Regulatory compliance: Adapting to frequent changes in billing and coding rules.
Claim denials and rejections: Due to incorrect coding or missing information.
Patient financial responsibility confusion: Lack of clarity about their share of the cost.
AR delays: Long payment cycles causing cash flow issues.
Regulatory compliance: Adapting to frequent changes in billing and coding rules.
Claim denials and rejections: Due to incorrect coding or missing information.
Patient financial responsibility confusion: Lack of clarity about their share of the cost.
AR delays: Long payment cycles causing cash flow issues.
Regulatory compliance: Adapting to frequent changes in billing and coding rules.
Claim denials and rejections: Due to incorrect coding or missing information.
Patient financial responsibility confusion: Lack of clarity about their share of the cost.
AR delays: Long payment cycles causing cash flow issues.
Regulatory compliance: Adapting to frequent changes in billing and coding rules.
09
Benefits of Outsourcing Medical Billing
09
Benefits of Outsourcing Medical Billing
09
Benefits of Outsourcing Medical Billing
09
Benefits of Outsourcing Medical Billing
Given the above challenges, outsourcing medical billing to experts offers several advantages:
Expertise and Accuracy: Professionals are trained in the latest coding and compliance standards.
Time Efficiency: Reduces administrative workload, freeing doctors to focus on patient care.
Improved Cash Flow: Speeds up reimbursement cycles and reduces denied claims.
Cost-Effectiveness: Eliminates the need for in-house staff, training, and technology investments.
Scalability: Adapts to the needs of growing practices, allowing doctors to focus on expansion.
Outsourcing medical billing not only addresses the challenges doctors face but also provides a streamlined, reliable solution for optimizing revenue cycles and minimizing stress. This makes it an invaluable strategy for modern healthcare practices.
Given the above challenges, outsourcing medical billing to experts offers several advantages:
Expertise and Accuracy: Professionals are trained in the latest coding and compliance standards.
Time Efficiency: Reduces administrative workload, freeing doctors to focus on patient care.
Improved Cash Flow: Speeds up reimbursement cycles and reduces denied claims.
Cost-Effectiveness: Eliminates the need for in-house staff, training, and technology investments.
Scalability: Adapts to the needs of growing practices, allowing doctors to focus on expansion.
Outsourcing medical billing not only addresses the challenges doctors face but also provides a streamlined, reliable solution for optimizing revenue cycles and minimizing stress. This makes it an invaluable strategy for modern healthcare practices.
Given the above challenges, outsourcing medical billing to experts offers several advantages:
Expertise and Accuracy: Professionals are trained in the latest coding and compliance standards.
Time Efficiency: Reduces administrative workload, freeing doctors to focus on patient care.
Improved Cash Flow: Speeds up reimbursement cycles and reduces denied claims.
Cost-Effectiveness: Eliminates the need for in-house staff, training, and technology investments.
Scalability: Adapts to the needs of growing practices, allowing doctors to focus on expansion.
Outsourcing medical billing not only addresses the challenges doctors face but also provides a streamlined, reliable solution for optimizing revenue cycles and minimizing stress. This makes it an invaluable strategy for modern healthcare practices.
Given the above challenges, outsourcing medical billing to experts offers several advantages:
Expertise and Accuracy: Professionals are trained in the latest coding and compliance standards.
Time Efficiency: Reduces administrative workload, freeing doctors to focus on patient care.
Improved Cash Flow: Speeds up reimbursement cycles and reduces denied claims.
Cost-Effectiveness: Eliminates the need for in-house staff, training, and technology investments.
Scalability: Adapts to the needs of growing practices, allowing doctors to focus on expansion.
Outsourcing medical billing not only addresses the challenges doctors face but also provides a streamlined, reliable solution for optimizing revenue cycles and minimizing stress. This makes it an invaluable strategy for modern healthcare practices.
Outsourcing Fees by Specialty
Explanation:
Billing System Monthly Costs: These are the costs for using in-house billing software, which may include claim submission, coding, and reporting tools.
Outsourcing Fees: Practices that choose to outsource their billing usually pay a percentage of the collections made, ranging from 4-7% depending on the specialty and billing company.
Sources for billing cost data:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by Specialty
Explanation:
Billing System Monthly Costs: These are the costs for using in-house billing software, which may include claim submission, coding, and reporting tools.
Outsourcing Fees: Practices that choose to outsource their billing usually pay a percentage of the collections made, ranging from 4-7% depending on the specialty and billing company.
Sources for billing cost data:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by Specialty
Explanation:
Billing System Monthly Costs: These are the costs for using in-house billing software, which may include claim submission, coding, and reporting tools.
Outsourcing Fees: Practices that choose to outsource their billing usually pay a percentage of the collections made, ranging from 4-7% depending on the specialty and billing company.
Sources for billing cost data:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by Specialty
Explanation:
Billing System Monthly Costs: These are the costs for using in-house billing software, which may include claim submission, coding, and reporting tools.
Outsourcing Fees: Practices that choose to outsource their billing usually pay a percentage of the collections made, ranging from 4-7% depending on the specialty and billing company.
Sources for billing cost data:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
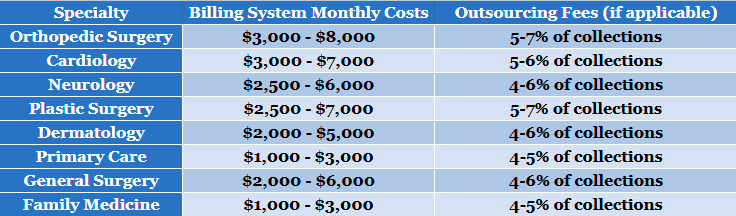



Outsourcing Fees by State:
Explanation:
Billing System Monthly Costs: Costs for maintaining an in-house billing system, including software, administrative support, and other related expenses.
Outsourcing Fees: A percentage of the revenue collected by billing companies. This varies based on the state's market and the complexity of the specialty.
Sources:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by State:
Explanation:
Billing System Monthly Costs: Costs for maintaining an in-house billing system, including software, administrative support, and other related expenses.
Outsourcing Fees: A percentage of the revenue collected by billing companies. This varies based on the state's market and the complexity of the specialty.
Sources:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by State:
Explanation:
Billing System Monthly Costs: Costs for maintaining an in-house billing system, including software, administrative support, and other related expenses.
Outsourcing Fees: A percentage of the revenue collected by billing companies. This varies based on the state's market and the complexity of the specialty.
Sources:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
Outsourcing Fees by State:
Explanation:
Billing System Monthly Costs: Costs for maintaining an in-house billing system, including software, administrative support, and other related expenses.
Outsourcing Fees: A percentage of the revenue collected by billing companies. This varies based on the state's market and the complexity of the specialty.
Sources:
Weatherby Healthcare:
https://www.weatherbyhealthcare.com
American Medical Association (AMA):
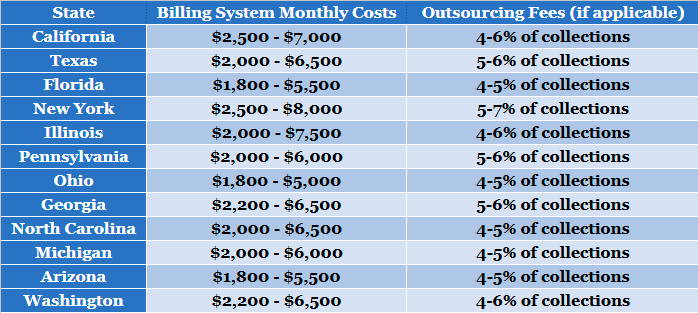



Notes:
Number of Practices Outsourcing: Estimates based on general trends in outsourcing medical billing and can vary by region within the state.
Outsourcing Providers: The percentage of practices that choose to outsource billing has been growing across the U.S., with some states (such as New York, California, and Florida) having higher adoption rates.
For more detailed data on outsourcing practices by state, you can refer to:
These sources offer comprehensive insights into billing practices, outsourcing adoption, and market trends across states.
Notes:
Number of Practices Outsourcing: Estimates based on general trends in outsourcing medical billing and can vary by region within the state.
Outsourcing Providers: The percentage of practices that choose to outsource billing has been growing across the U.S., with some states (such as New York, California, and Florida) having higher adoption rates.
For more detailed data on outsourcing practices by state, you can refer to:
These sources offer comprehensive insights into billing practices, outsourcing adoption, and market trends across states.
Notes:
Number of Practices Outsourcing: Estimates based on general trends in outsourcing medical billing and can vary by region within the state.
Outsourcing Providers: The percentage of practices that choose to outsource billing has been growing across the U.S., with some states (such as New York, California, and Florida) having higher adoption rates.
For more detailed data on outsourcing practices by state, you can refer to:
These sources offer comprehensive insights into billing practices, outsourcing adoption, and market trends across states.
Notes:
Number of Practices Outsourcing: Estimates based on general trends in outsourcing medical billing and can vary by region within the state.
Outsourcing Providers: The percentage of practices that choose to outsource billing has been growing across the U.S., with some states (such as New York, California, and Florida) having higher adoption rates.
For more detailed data on outsourcing practices by state, you can refer to:
These sources offer comprehensive insights into billing practices, outsourcing adoption, and market trends across states.
10
Target Market Analysis
10
Target Market Analysis
10
Target Market Analysis
10
Target Market Analysis
Number of Physicians by State (2021 Estimates)
Key Insights:
1.States with the Most Doctors:
California (130,000), New York (100,000), and Texas (80,000).
These states also have extensive healthcare systems and demand for specialists.
2.States with the Fewest Doctors:
Wyoming (3,000) and Vermont (3,500), due to smaller populations.
3.Dominant Specialties:
Psychiatry, Surgery, and Family Medicine dominate in larger states.
Family Medicine is crucial in rural areas like Wyoming and Alaska.
Number of Physicians by State (2021 Estimates)
Key Insights:
1.States with the Most Doctors:
California (130,000), New York (100,000), and Texas (80,000).
These states also have extensive healthcare systems and demand for specialists.
2.States with the Fewest Doctors:
Wyoming (3,000) and Vermont (3,500), due to smaller populations.
3.Dominant Specialties:
Psychiatry, Surgery, and Family Medicine dominate in larger states.
Family Medicine is crucial in rural areas like Wyoming and Alaska.
Number of Physicians by State (2021 Estimates)
Key Insights:
1.States with the Most Doctors:
California (130,000), New York (100,000), and Texas (80,000).
These states also have extensive healthcare systems and demand for specialists.
2.States with the Fewest Doctors:
Wyoming (3,000) and Vermont (3,500), due to smaller populations.
3.Dominant Specialties:
Psychiatry, Surgery, and Family Medicine dominate in larger states.
Family Medicine is crucial in rural areas like Wyoming and Alaska.
Number of Physicians by State (2021 Estimates)
Key Insights:
1.States with the Most Doctors:
California (130,000), New York (100,000), and Texas (80,000).
These states also have extensive healthcare systems and demand for specialists.
2.States with the Fewest Doctors:
Wyoming (3,000) and Vermont (3,500), due to smaller populations.
3.Dominant Specialties:
Psychiatry, Surgery, and Family Medicine dominate in larger states.
Family Medicine is crucial in rural areas like Wyoming and Alaska.
References:
1.AAMC's State Physician Workforce Data Report 2021
Provides extensive details about the number of active physicians, their specialties, and state-wise distribution.
URL: https://www.aamc.org/data-reports/workforce/report/state-physician-workforce-data-report
2.Statista - Number of Active Physicians in the U.S. (2021)
Offers statistical insights on the distribution of primary care and specialty physicians across U.S. states.
URL: https://www.statista.com/statistics/236593/number-of-active-physicians-in-the-us-by-state/
References:
1.AAMC's State Physician Workforce Data Report 2021
Provides extensive details about the number of active physicians, their specialties, and state-wise distribution.
URL: https://www.aamc.org/data-reports/workforce/report/state-physician-workforce-data-report
2.Statista - Number of Active Physicians in the U.S. (2021)
Offers statistical insights on the distribution of primary care and specialty physicians across U.S. states.
URL: https://www.statista.com/statistics/236593/number-of-active-physicians-in-the-us-by-state/
References:
1.AAMC's State Physician Workforce Data Report 2021
Provides extensive details about the number of active physicians, their specialties, and state-wise distribution.
URL: https://www.aamc.org/data-reports/workforce/report/state-physician-workforce-data-report
2.Statista - Number of Active Physicians in the U.S. (2021)
Offers statistical insights on the distribution of primary care and specialty physicians across U.S. states.
URL: https://www.statista.com/statistics/236593/number-of-active-physicians-in-the-us-by-state/
References:
1.AAMC's State Physician Workforce Data Report 2021
Provides extensive details about the number of active physicians, their specialties, and state-wise distribution.
URL: https://www.aamc.org/data-reports/workforce/report/state-physician-workforce-data-report
2.Statista - Number of Active Physicians in the U.S. (2021)
Offers statistical insights on the distribution of primary care and specialty physicians across U.S. states.
URL: https://www.statista.com/statistics/236593/number-of-active-physicians-in-the-us-by-state/
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
Specialty Based Average Revenue for various types of Practices:
Key Insights:
Highest Earners: Orthopedic surgeons and cardiologists continue to be the highest earners in both annual and monthly revenue.
Self-Employed vs Employed: Physicians in private practices tend to earn more on a monthly basis compared to their employed counterparts.
Rural vs Urban Settings: Physicians in rural settings typically have higher monthly earnings due to lower operational costs and less competition.
References:
Weatherby Healthcare. (2024). "Physician salary report: Results show increased earnings."
Retrieved from: https://www.weatherbyhealthcare.com.
American Medical Association (AMA). (2024). "State Physician Workforce Data."
Retrieved from: https://www.ama-assn.org.
References:
Weatherby Healthcare. (2024). "Physician salary report: Results show increased earnings."
Retrieved from: https://www.weatherbyhealthcare.com.
American Medical Association (AMA). (2024). "State Physician Workforce Data."
Retrieved from: https://www.ama-assn.org.
References:
Weatherby Healthcare. (2024). "Physician salary report: Results show increased earnings."
Retrieved from: https://www.weatherbyhealthcare.com.
American Medical Association (AMA). (2024). "State Physician Workforce Data."
Retrieved from: https://www.ama-assn.org.
References:
Weatherby Healthcare. (2024). "Physician salary report: Results show increased earnings."
Retrieved from: https://www.weatherbyhealthcare.com.
American Medical Association (AMA). (2024). "State Physician Workforce Data."
Retrieved from: https://www.ama-assn.org.
11
Cost-Benefit Analysis
11
Cost-Benefit Analysis
11
Cost-Benefit Analysis
11
Cost-Benefit Analysis
In-House Vs Outsourced:
The amount healthcare practices save by outsourcing medical billing varies depending on their size, patient volume, and the complexity of their billing needs. However, outsourcing typically results in significant cost reductions, improved cash flow, and fewer denied claims. Here’s a detailed breakdown of how savings are realized and quantified:
In-House Vs Outsourced:
The amount healthcare practices save by outsourcing medical billing varies depending on their size, patient volume, and the complexity of their billing needs. However, outsourcing typically results in significant cost reductions, improved cash flow, and fewer denied claims. Here’s a detailed breakdown of how savings are realized and quantified:
In-House Vs Outsourced:
The amount healthcare practices save by outsourcing medical billing varies depending on their size, patient volume, and the complexity of their billing needs. However, outsourcing typically results in significant cost reductions, improved cash flow, and fewer denied claims. Here’s a detailed breakdown of how savings are realized and quantified:
In-House Vs Outsourced:
The amount healthcare practices save by outsourcing medical billing varies depending on their size, patient volume, and the complexity of their billing needs. However, outsourcing typically results in significant cost reductions, improved cash flow, and fewer denied claims. Here’s a detailed breakdown of how savings are realized and quantified:
1. Cost of In-House Billing
Staffing Costs
Salaries and Benefits: Employing in-house billing staff can cost between $40,000 and $70,000 annually per staff member, depending on experience and location. Practices often need multiple billers for larger workloads.
Training Expenses: Regular training for staff to stay updated with regulatory changes and coding requirements can cost several thousand dollars annually.
Overhead Costs
Office Space and Supplies: Maintaining an in-house billing team requires dedicated office space, computers, software, and supplies, adding $15,000–$25,000 annually per employee.
Technology Investments
Billing Software: Subscription fees for billing software can range from $3,000 to $7,000 annually, with additional costs for updates and integrations.
Cybersecurity: Securing patient data adds $5,000–$15,000 annually in IT expenses.
1. Cost of In-House Billing
Staffing Costs
Salaries and Benefits: Employing in-house billing staff can cost between $40,000 and $70,000 annually per staff member, depending on experience and location. Practices often need multiple billers for larger workloads.
Training Expenses: Regular training for staff to stay updated with regulatory changes and coding requirements can cost several thousand dollars annually.
Overhead Costs
Office Space and Supplies: Maintaining an in-house billing team requires dedicated office space, computers, software, and supplies, adding $15,000–$25,000 annually per employee.
Technology Investments
Billing Software: Subscription fees for billing software can range from $3,000 to $7,000 annually, with additional costs for updates and integrations.
Cybersecurity: Securing patient data adds $5,000–$15,000 annually in IT expenses.
1. Cost of In-House Billing
Staffing Costs
Salaries and Benefits: Employing in-house billing staff can cost between $40,000 and $70,000 annually per staff member, depending on experience and location. Practices often need multiple billers for larger workloads.
Training Expenses: Regular training for staff to stay updated with regulatory changes and coding requirements can cost several thousand dollars annually.
Overhead Costs
Office Space and Supplies: Maintaining an in-house billing team requires dedicated office space, computers, software, and supplies, adding $15,000–$25,000 annually per employee.
Technology Investments
Billing Software: Subscription fees for billing software can range from $3,000 to $7,000 annually, with additional costs for updates and integrations.
Cybersecurity: Securing patient data adds $5,000–$15,000 annually in IT expenses.
1. Cost of In-House Billing
Staffing Costs
Salaries and Benefits: Employing in-house billing staff can cost between $40,000 and $70,000 annually per staff member, depending on experience and location. Practices often need multiple billers for larger workloads.
Training Expenses: Regular training for staff to stay updated with regulatory changes and coding requirements can cost several thousand dollars annually.
Overhead Costs
Office Space and Supplies: Maintaining an in-house billing team requires dedicated office space, computers, software, and supplies, adding $15,000–$25,000 annually per employee.
Technology Investments
Billing Software: Subscription fees for billing software can range from $3,000 to $7,000 annually, with additional costs for updates and integrations.
Cybersecurity: Securing patient data adds $5,000–$15,000 annually in IT expenses.
2. Savings from Outsourcing
Outsourcing eliminates or significantly reduces many of these costs, typically offering billing services for 4–7% of total collections. Here's a comparison:
2.1.Small Practice Example
Annual Revenue: $500,000
In-House Billing Costs: $70,000–$100,000 (staff, software, and overhead)
Outsourcing Cost: $20,000–$35,000 (4–7% of revenue)
Savings: $50,000–$80,000 annually
2.2.Medium-Sized Practice Example
Annual Revenue: $1,500,000
In-House Billing Costs: $150,000–$200,000
Outsourcing Cost: $60,000–$105,000
Savings: $90,000–$140,000 annually
2.3.Large Practice Example
Annual Revenue: $5,000,000
In-House Billing Costs: $500,000+
Outsourcing Cost: $200,000–$350,000
Savings: $150,000–$300,000 annually
2. Savings from Outsourcing
Outsourcing eliminates or significantly reduces many of these costs, typically offering billing services for 4–7% of total collections. Here's a comparison:
2.1.Small Practice Example
Annual Revenue: $500,000
In-House Billing Costs: $70,000–$100,000 (staff, software, and overhead)
Outsourcing Cost: $20,000–$35,000 (4–7% of revenue)
Savings: $50,000–$80,000 annually
2.2.Medium-Sized Practice Example
Annual Revenue: $1,500,000
In-House Billing Costs: $150,000–$200,000
Outsourcing Cost: $60,000–$105,000
Savings: $90,000–$140,000 annually
2.3.Large Practice Example
Annual Revenue: $5,000,000
In-House Billing Costs: $500,000+
Outsourcing Cost: $200,000–$350,000
Savings: $150,000–$300,000 annually
2. Savings from Outsourcing
Outsourcing eliminates or significantly reduces many of these costs, typically offering billing services for 4–7% of total collections. Here's a comparison:
2.1.Small Practice Example
Annual Revenue: $500,000
In-House Billing Costs: $70,000–$100,000 (staff, software, and overhead)
Outsourcing Cost: $20,000–$35,000 (4–7% of revenue)
Savings: $50,000–$80,000 annually
2.2.Medium-Sized Practice Example
Annual Revenue: $1,500,000
In-House Billing Costs: $150,000–$200,000
Outsourcing Cost: $60,000–$105,000
Savings: $90,000–$140,000 annually
2.3.Large Practice Example
Annual Revenue: $5,000,000
In-House Billing Costs: $500,000+
Outsourcing Cost: $200,000–$350,000
Savings: $150,000–$300,000 annually
2. Savings from Outsourcing
Outsourcing eliminates or significantly reduces many of these costs, typically offering billing services for 4–7% of total collections. Here's a comparison:
2.1.Small Practice Example
Annual Revenue: $500,000
In-House Billing Costs: $70,000–$100,000 (staff, software, and overhead)
Outsourcing Cost: $20,000–$35,000 (4–7% of revenue)
Savings: $50,000–$80,000 annually
2.2.Medium-Sized Practice Example
Annual Revenue: $1,500,000
In-House Billing Costs: $150,000–$200,000
Outsourcing Cost: $60,000–$105,000
Savings: $90,000–$140,000 annually
2.3.Large Practice Example
Annual Revenue: $5,000,000
In-House Billing Costs: $500,000+
Outsourcing Cost: $200,000–$350,000
Savings: $150,000–$300,000 annually
3. Additional Financial Benefits
1.Reduced Denied Claims: Experts reduce claim errors, leading to faster reimbursements and fewer lost revenues, which can add up to 10–15% of potential collections.
2.Faster Cash Flow: Outsourcing firms often expedite claim submissions and follow-ups, reducing days in accounts receivable (AR) and improving practice liquidity.
3.Avoiding Hidden Costs: Practices save on recruiting, onboarding, training, and replacing staff, which can be a significant recurring expense.
4.Compliance Avoidance Costs: Outsourcing minimizes risks of costly fines and audits due to non-compliance with billing regulations.
3. Additional Financial Benefits
1.Reduced Denied Claims: Experts reduce claim errors, leading to faster reimbursements and fewer lost revenues, which can add up to 10–15% of potential collections.
2.Faster Cash Flow: Outsourcing firms often expedite claim submissions and follow-ups, reducing days in accounts receivable (AR) and improving practice liquidity.
3.Avoiding Hidden Costs: Practices save on recruiting, onboarding, training, and replacing staff, which can be a significant recurring expense.
4.Compliance Avoidance Costs: Outsourcing minimizes risks of costly fines and audits due to non-compliance with billing regulations.
3. Additional Financial Benefits
1.Reduced Denied Claims: Experts reduce claim errors, leading to faster reimbursements and fewer lost revenues, which can add up to 10–15% of potential collections.
2.Faster Cash Flow: Outsourcing firms often expedite claim submissions and follow-ups, reducing days in accounts receivable (AR) and improving practice liquidity.
3.Avoiding Hidden Costs: Practices save on recruiting, onboarding, training, and replacing staff, which can be a significant recurring expense.
4.Compliance Avoidance Costs: Outsourcing minimizes risks of costly fines and audits due to non-compliance with billing regulations.
3. Additional Financial Benefits
1.Reduced Denied Claims: Experts reduce claim errors, leading to faster reimbursements and fewer lost revenues, which can add up to 10–15% of potential collections.
2.Faster Cash Flow: Outsourcing firms often expedite claim submissions and follow-ups, reducing days in accounts receivable (AR) and improving practice liquidity.
3.Avoiding Hidden Costs: Practices save on recruiting, onboarding, training, and replacing staff, which can be a significant recurring expense.
4.Compliance Avoidance Costs: Outsourcing minimizes risks of costly fines and audits due to non-compliance with billing regulations.
4. Total Impact
Over time, outsourcing medical billing can save 20–40% of total administrative costs while also increasing collections by 10–20%, offering a dual advantage of cost reduction and revenue growth. This makes outsourcing an attractive option for practices looking to optimize their financial health and focus on patient care.
4. Total Impact
Over time, outsourcing medical billing can save 20–40% of total administrative costs while also increasing collections by 10–20%, offering a dual advantage of cost reduction and revenue growth. This makes outsourcing an attractive option for practices looking to optimize their financial health and focus on patient care.
4. Total Impact
Over time, outsourcing medical billing can save 20–40% of total administrative costs while also increasing collections by 10–20%, offering a dual advantage of cost reduction and revenue growth. This makes outsourcing an attractive option for practices looking to optimize their financial health and focus on patient care.
4. Total Impact
Over time, outsourcing medical billing can save 20–40% of total administrative costs while also increasing collections by 10–20%, offering a dual advantage of cost reduction and revenue growth. This makes outsourcing an attractive option for practices looking to optimize their financial health and focus on patient care.
Financial Benefits from Outsourcing:
1.Reduced Denied Claims: Outsourcing reduces claim errors, leading to faster reimbursements and fewer lost revenues, potentially saving 10-15% of collections.
2.Faster Cash Flow: Outsourced billing firms expedite claim submissions and follow-ups, reducing days in accounts receivable and improving liquidity.
3.Avoiding Hidden Costs: Practices save on recruitment, onboarding, training, and replacing staff, which are significant recurring expenses.
4.Compliance Avoidance Costs: Minimizing the risk of costly fines and audits due to non-compliance with billing regulations.
Total Impact:
Savings: Over time, practices can save 20-40% of total administrative costs by outsourcing billing, and collections may improve by 10-20%.
Revenue Growth: Outsourcing offers the dual benefit of reducing costs and increasing revenue, helping practices optimize financial health.
This data is based on industry averages, and specific savings can vary depending on a practice’s unique situation, including the volume of claims, complexity, and operational structure.
Sources:
Financial Benefits from Outsourcing:
1.Reduced Denied Claims: Outsourcing reduces claim errors, leading to faster reimbursements and fewer lost revenues, potentially saving 10-15% of collections.
2.Faster Cash Flow: Outsourced billing firms expedite claim submissions and follow-ups, reducing days in accounts receivable and improving liquidity.
3.Avoiding Hidden Costs: Practices save on recruitment, onboarding, training, and replacing staff, which are significant recurring expenses.
4.Compliance Avoidance Costs: Minimizing the risk of costly fines and audits due to non-compliance with billing regulations.
Total Impact:
Savings: Over time, practices can save 20-40% of total administrative costs by outsourcing billing, and collections may improve by 10-20%.
Revenue Growth: Outsourcing offers the dual benefit of reducing costs and increasing revenue, helping practices optimize financial health.
This data is based on industry averages, and specific savings can vary depending on a practice’s unique situation, including the volume of claims, complexity, and operational structure.
Sources:
Financial Benefits from Outsourcing:
1.Reduced Denied Claims: Outsourcing reduces claim errors, leading to faster reimbursements and fewer lost revenues, potentially saving 10-15% of collections.
2.Faster Cash Flow: Outsourced billing firms expedite claim submissions and follow-ups, reducing days in accounts receivable and improving liquidity.
3.Avoiding Hidden Costs: Practices save on recruitment, onboarding, training, and replacing staff, which are significant recurring expenses.
4.Compliance Avoidance Costs: Minimizing the risk of costly fines and audits due to non-compliance with billing regulations.
Total Impact:
Savings: Over time, practices can save 20-40% of total administrative costs by outsourcing billing, and collections may improve by 10-20%.
Revenue Growth: Outsourcing offers the dual benefit of reducing costs and increasing revenue, helping practices optimize financial health.
This data is based on industry averages, and specific savings can vary depending on a practice’s unique situation, including the volume of claims, complexity, and operational structure.
Sources:
Financial Benefits from Outsourcing:
1.Reduced Denied Claims: Outsourcing reduces claim errors, leading to faster reimbursements and fewer lost revenues, potentially saving 10-15% of collections.
2.Faster Cash Flow: Outsourced billing firms expedite claim submissions and follow-ups, reducing days in accounts receivable and improving liquidity.
3.Avoiding Hidden Costs: Practices save on recruitment, onboarding, training, and replacing staff, which are significant recurring expenses.
4.Compliance Avoidance Costs: Minimizing the risk of costly fines and audits due to non-compliance with billing regulations.
Total Impact:
Savings: Over time, practices can save 20-40% of total administrative costs by outsourcing billing, and collections may improve by 10-20%.
Revenue Growth: Outsourcing offers the dual benefit of reducing costs and increasing revenue, helping practices optimize financial health.
This data is based on industry averages, and specific savings can vary depending on a practice’s unique situation, including the volume of claims, complexity, and operational structure.
Sources:
12
Pricing Strategy
12
Pricing Strategy
12
Pricing Strategy
12
Pricing Strategy
<$30,000 Revenue
We charge percentage fees of
6%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benifits)
Prior Authorization
24/7 email support
<$30,000 Revenue
We charge percentage fees of
6%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benifits)
Prior Authorization
24/7 email support
<$30,000 Revenue
We charge percentage fees of
6%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benifits)
Prior Authorization
24/7 email support
<$30,000 Revenue
We charge percentage fees of
6%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benifits)
Prior Authorization
24/7 email support
$31,000 - $100,000 Revenue
We charge percentage of
5%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$31,000 - $100,000 Revenue
We charge percentage of
5%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$31,000 - $100,000 Revenue
We charge percentage of
5%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$31,000 - $100,000 Revenue
We charge percentage of
5%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$101,000-$150,000 Revenue
We charge percentage of
4%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$101,000-$150,000 Revenue
We charge percentage of
4%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$101,000-$150,000 Revenue
We charge percentage of
4%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
$101,000-$150,000 Revenue
We charge percentage of
4%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
>$150,000 Revenue
We charge percentage of
3%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
>$150,000 Revenue
We charge percentage of
3%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
>$150,000 Revenue
We charge percentage of
3%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
>$150,000 Revenue
We charge percentage of
3%
/month (negotiable)
Front Desk Support
Charge Entry
AR Management
Payment Posting
Credentialing Services
Coding
VOB(Verification of Benefits)
Prior Authorization
Priority email and phone support
13
Financial Dashboard
13
Financial Dashboard
13
Financial Dashboard
13
Financial Dashboard
Introduction:
At My Health Aiyin, we understand the challenges that come with managing the financial aspects of a dental practice. To address these challenges and provide complete transparency, we've developed a dedicated portal for doctors. This portal allows you to have full visibility of our progress and your practice's financial health, without relying on your practice management system or employees.
Introduction:
At My Health Aiyin, we understand the challenges that come with managing the financial aspects of a dental practice. To address these challenges and provide complete transparency, we've developed a dedicated portal for doctors. This portal allows you to have full visibility of our progress and your practice's financial health, without relying on your practice management system or employees.
Introduction:
At My Health Aiyin, we understand the challenges that come with managing the financial aspects of a dental practice. To address these challenges and provide complete transparency, we've developed a dedicated portal for doctors. This portal allows you to have full visibility of our progress and your practice's financial health, without relying on your practice management system or employees.
Introduction:
At My Health Aiyin, we understand the challenges that come with managing the financial aspects of a dental practice. To address these challenges and provide complete transparency, we've developed a dedicated portal for doctors. This portal allows you to have full visibility of our progress and your practice's financial health, without relying on your practice management system or employees.
Unique Selling Value:
1. Comprehensive Practice Reporting:
Generate Comprehensive Practice Report: Easily generate structured PDF reports that consolidate your financial and claims data for offline review. This feature ensures you have a clear and organized record of your practice's performance.
2. Real-Time Claims Reporting:
Claims Aging and Status: Access detailed reports showing the number of claims and their aging brackets (0-30 days, 31-60days, 61-90 days, over 90 days). This helps you understand where delays might be happening and take necessary actions to expedite payments.
Balance Reporting: View your total balance along with breakdowns by aging bracket. This helps you manage outstanding balances and prioritize follow-ups for older claims.
3. Payment and Denial Tracking:
Paid Status: A clear visual representation of the paid amount versus the number of paid claims. This allows you to track payments received efficiently.
Denial and Resubmission Management: Track denied claims, resubmitted claims, and the associated amounts. This ensures you are aware of all pending and resubmitted claims, helping you take corrective actions swiftly.
4. Insurance-Wise Reporting:
Insurance Specific Reports: Get detailed insights into claims and balances by specific insurance providers. This enables you to identify patterns or issues with particular insurers and address them promptly.
5. Status Reporting:
Patient Responsibility and Adjustments: View the total patient responsibility and the number of claims adjusted or written off. This provides a comprehensive view of patient payments and adjustments, helping you manage patient billing effectively.
Appeals and Reconciliations: Keep track of the number of appeals and reconciliations. This ensures you stay informed about the progress of disputed claims and their resolutions.
Unique Selling Value:
1. Comprehensive Practice Reporting:
Generate Comprehensive Practice Report: Easily generate structured PDF reports that consolidate your financial and claims data for offline review. This feature ensures you have a clear and organized record of your practice's performance.
2. Real-Time Claims Reporting:
Claims Aging and Status: Access detailed reports showing the number of claims and their aging brackets (0-30 days, 31-60days, 61-90 days, over 90 days). This helps you understand where delays might be happening and take necessary actions to expedite payments.
Balance Reporting: View your total balance along with breakdowns by aging bracket. This helps you manage outstanding balances and prioritize follow-ups for older claims.
3. Payment and Denial Tracking:
Paid Status: A clear visual representation of the paid amount versus the number of paid claims. This allows you to track payments received efficiently.
Denial and Resubmission Management: Track denied claims, resubmitted claims, and the associated amounts. This ensures you are aware of all pending and resubmitted claims, helping you take corrective actions swiftly.
4. Insurance-Wise Reporting:
Insurance Specific Reports: Get detailed insights into claims and balances by specific insurance providers. This enables you to identify patterns or issues with particular insurers and address them promptly.
5. Status Reporting:
Patient Responsibility and Adjustments: View the total patient responsibility and the number of claims adjusted or written off. This provides a comprehensive view of patient payments and adjustments, helping you manage patient billing effectively.
Appeals and Reconciliations: Keep track of the number of appeals and reconciliations. This ensures you stay informed about the progress of disputed claims and their resolutions.
Unique Selling Value:
1. Comprehensive Practice Reporting:
Generate Comprehensive Practice Report: Easily generate structured PDF reports that consolidate your financial and claims data for offline review. This feature ensures you have a clear and organized record of your practice's performance.
2. Real-Time Claims Reporting:
Claims Aging and Status: Access detailed reports showing the number of claims and their aging brackets (0-30 days, 31-60days, 61-90 days, over 90 days). This helps you understand where delays might be happening and take necessary actions to expedite payments.
Balance Reporting: View your total balance along with breakdowns by aging bracket. This helps you manage outstanding balances and prioritize follow-ups for older claims.
3. Payment and Denial Tracking:
Paid Status: A clear visual representation of the paid amount versus the number of paid claims. This allows you to track payments received efficiently.
Denial and Resubmission Management: Track denied claims, resubmitted claims, and the associated amounts. This ensures you are aware of all pending and resubmitted claims, helping you take corrective actions swiftly.
4. Insurance-Wise Reporting:
Insurance Specific Reports: Get detailed insights into claims and balances by specific insurance providers. This enables you to identify patterns or issues with particular insurers and address them promptly.
5. Status Reporting:
Patient Responsibility and Adjustments: View the total patient responsibility and the number of claims adjusted or written off. This provides a comprehensive view of patient payments and adjustments, helping you manage patient billing effectively.
Appeals and Reconciliations: Keep track of the number of appeals and reconciliations. This ensures you stay informed about the progress of disputed claims and their resolutions.
Unique Selling Value:
1. Comprehensive Practice Reporting:
Generate Comprehensive Practice Report: Easily generate structured PDF reports that consolidate your financial and claims data for offline review. This feature ensures you have a clear and organized record of your practice's performance.
2. Real-Time Claims Reporting:
Claims Aging and Status: Access detailed reports showing the number of claims and their aging brackets (0-30 days, 31-60days, 61-90 days, over 90 days). This helps you understand where delays might be happening and take necessary actions to expedite payments.
Balance Reporting: View your total balance along with breakdowns by aging bracket. This helps you manage outstanding balances and prioritize follow-ups for older claims.
3. Payment and Denial Tracking:
Paid Status: A clear visual representation of the paid amount versus the number of paid claims. This allows you to track payments received efficiently.
Denial and Resubmission Management: Track denied claims, resubmitted claims, and the associated amounts. This ensures you are aware of all pending and resubmitted claims, helping you take corrective actions swiftly.
4. Insurance-Wise Reporting:
Insurance Specific Reports: Get detailed insights into claims and balances by specific insurance providers. This enables you to identify patterns or issues with particular insurers and address them promptly.
5. Status Reporting:
Patient Responsibility and Adjustments: View the total patient responsibility and the number of claims adjusted or written off. This provides a comprehensive view of patient payments and adjustments, helping you manage patient billing effectively.
Appeals and Reconciliations: Keep track of the number of appeals and reconciliations. This ensures you stay informed about the progress of disputed claims and their resolutions.
Impact on Your Practice:
Transparency and Control: The portal provides complete transparency, allowing you to stay informed about all financial transactions and claims processing activities. This reduces dependency on practice management systems and employees.
Improved Cash Flow Management: By having real-time access to claims status, payments, and outstanding balances, you can better manage your cash flow and financial planning.
Efficient Issue Resolution: The detailed reporting on denials, resubmissions, and appeals helps you quickly identify and address issues, reducing delays in payments.
Better Decision Making: With comprehensive and up-to-date data at your fingertips, you can make informed decisions to enhance the financial performance of your practice.
Impact on Your Practice:
Transparency and Control: The portal provides complete transparency, allowing you to stay informed about all financial transactions and claims processing activities. This reduces dependency on practice management systems and employees.
Improved Cash Flow Management: By having real-time access to claims status, payments, and outstanding balances, you can better manage your cash flow and financial planning.
Efficient Issue Resolution: The detailed reporting on denials, resubmissions, and appeals helps you quickly identify and address issues, reducing delays in payments.
Better Decision Making: With comprehensive and up-to-date data at your fingertips, you can make informed decisions to enhance the financial performance of your practice.
Impact on Your Practice:
Transparency and Control: The portal provides complete transparency, allowing you to stay informed about all financial transactions and claims processing activities. This reduces dependency on practice management systems and employees.
Improved Cash Flow Management: By having real-time access to claims status, payments, and outstanding balances, you can better manage your cash flow and financial planning.
Efficient Issue Resolution: The detailed reporting on denials, resubmissions, and appeals helps you quickly identify and address issues, reducing delays in payments.
Better Decision Making: With comprehensive and up-to-date data at your fingertips, you can make informed decisions to enhance the financial performance of your practice.
Impact on Your Practice:
Transparency and Control: The portal provides complete transparency, allowing you to stay informed about all financial transactions and claims processing activities. This reduces dependency on practice management systems and employees.
Improved Cash Flow Management: By having real-time access to claims status, payments, and outstanding balances, you can better manage your cash flow and financial planning.
Efficient Issue Resolution: The detailed reporting on denials, resubmissions, and appeals helps you quickly identify and address issues, reducing delays in payments.
Better Decision Making: With comprehensive and up-to-date data at your fingertips, you can make informed decisions to enhance the financial performance of your practice.
Client Portal Preview:
Below is a collage of the portal pages showcasing the various features and their benefits:
1. Comprehensive Practice Report Generation
2. Claims Reporting with Aging Brackets
3. Balance Reporting by Aging Bracket
4. Paid Status Visualization
5. Insurance-Wise Reporting
6. Patient Responsibility and Adjustments
7. Overall Financial Summary and Key Metrics
Client Portal Preview:
Below is a collage of the portal pages showcasing the various features and their benefits:
1. Comprehensive Practice Report Generation
2. Claims Reporting with Aging Brackets
3. Balance Reporting by Aging Bracket
4. Paid Status Visualization
5. Insurance-Wise Reporting
6. Patient Responsibility and Adjustments
7. Overall Financial Summary and Key Metrics
Client Portal Preview:
Below is a collage of the portal pages showcasing the various features and their benefits:
1. Comprehensive Practice Report Generation
2. Claims Reporting with Aging Brackets
3. Balance Reporting by Aging Bracket
4. Paid Status Visualization
5. Insurance-Wise Reporting
6. Patient Responsibility and Adjustments
7. Overall Financial Summary and Key Metrics
Client Portal Preview:
Below is a collage of the portal pages showcasing the various features and their benefits:
1. Comprehensive Practice Report Generation
2. Claims Reporting with Aging Brackets
3. Balance Reporting by Aging Bracket
4. Paid Status Visualization
5. Insurance-Wise Reporting
6. Patient Responsibility and Adjustments
7. Overall Financial Summary and Key Metrics
14
Call to Action
14
Call to Action
14
Call to Action
14
Call to Action
Are you a healthcare professional looking for reliable and efficient medical billing services? Let us help you focus on patient care while we handle your revenue cycle management with precision and compliance.
📞 Call Us Today
Get started by speaking with one of our billing experts. Call us at +1 (408) 600-0275 to learn more about how our solutions can improve your practice’s cash flow and reduce administrative burdens.
📧 Email Us
Have questions or need a customized proposal? Email us at myhealth.aiyin.us@gmail.com. We’re here to provide tailored solutions for your unique billing needs.
📍 Visit Us
We’re located at 1201 Parkmoor Ave, San Jose, CA, 95126, United States. Schedule a meeting with us to discuss how we can support your practice's financial health and operational efficiency.
Take the first step toward hassle-free medical billing—partner with My Health Aiyin and let us help your practice grow and thrive.
1. Precedence Research. (2024). U.S. Medical Billing Outsourcing Market Size, Growth, Report 2032. Retrieved from https://www.precedenceresearch.com/us-medical-billing-outsourcing-market
2. Outsource Accelerator. (2024). Why healthcare providers should outsource medical billing services. Retrieved from https://www.outsourceaccelerator.com/articles/outsource-medical-billing-services/
3. Purview Healthcare. (2024). What is Outsourcing Medical Billing: Pros & Cons Explained. Retrieved from https://purviewhealthcare.com/outsourcing-medical-billing-pros-and-cons/
4. Park Medical Billing. (2024). Advantages of Outsourcing Medical Billing vs. In-House Billers. Retrieved from https://www.parkmedicalbilling.com/advantages-of-outsourcing-medical-billing-vs-in-house-billers/
5. Global Market Insights. (2023). Medical Billing Outsourcing Market Size – Analysis Report, 2032. Retrieved from https://www.gminsights.com/industry-analysis/medical-billing-outsourcing-market
6. Fortune Business Insights. (2024). U.S. Medical Billing Outsourcing Market Size | Analysis [2030]. Retrieved from https://www.fortunebusinessinsights.com/u-s-medical-billing-outsourcing-market-109113
7. Dimension Market Research. (2024). U.S. Medical Billing Outsourcing Market Is Expected To Reach Revenue Of USD 16.9 Bn By 2033, At 12.5% CAGR. Retrieved from https://www.globenewswire.com/news-release/2024/11/19/2983846/0/en/U-S-Medical-Billing-Outsourcing-Market-Is-Expected-To-Reach-Revenue-Of-USD-16-9-Bn-By-2033-At-12-5-CAGR-Dimension-Market-Research.html
8. Outsource Strategies International. (2023). 6 Medical Billing Outsourcing Benefits for Healthcare Practices. Retrieved from https://www.outsourcestrategies.com/blog/benefits-of-outsourcing-medical-billing-services/
9. Future Market Insights. (2024). Medical Billing Outsourcing Market - Future Market Insights. Retrieved from https://www.futuremarketinsights.com/reports/medical-billing-outsourcing-market
10. IBN Technologies. (2024). 9 Benefits of Medical Billing Outsourcing. Retrieved from https://www.ibntech.com/blog/benefits-of-medical-billing-outsourcing/
11. Unity Connect. (2024). Benefits and Disadvantages of Outsourcing Medical Billing. Retrieved from https://unity-connect.com/our-resources/blog/outsourcing-medical-billing/
12. Research and Markets. (2024). U.S. Medical Billing Outsourcing Market Size & Competitors. Retrieved from https://www.researchandmarkets.com/report/united-states-medical-billing-outsourcing-market
13. Outsourcey. (2024). Top 10 Benefits of Outsourcing Medical Billing. Retrieved from https://outsourcey.com/learning-centre/top-10-benefits-of-outsourcing-medical-billing/
14. P&S Intelligence. (2024). Medical Billing Outsourcing Market Size Report, 2030. Retrieved from https://www.psmarketresearch.com/market-analysis/medical-billing-outsourcing-market-report
15. Human Medical Billing. (2024). 12 Benefits of Outsourcing Medical Billing Services for Providers. Retrieved from https://humanmedicalbilling.com/12-benefits-of-outsourcing-medical-billing-services-for-providers/
16. IMARC Group. (2024). United States Medical Billing Outsourcing Market. Retrieved from https://www.imarcgroup.com/united-states-medical-billing-outsourcing-market
17. Valerion Health. (2024). What Are The Benefits of Outsourcing Medical Billing?. Retrieved from https://valerionhealth.com/blog/benefits-of-outsourcing-medical-billing/
18. Wikipedia. (2024). Medical billing. Retrieved from https://en.wikipedia.org/wiki/Medical_billing
Are you a healthcare professional looking for reliable and efficient medical billing services? Let us help you focus on patient care while we handle your revenue cycle management with precision and compliance.
📞 Call Us Today
Get started by speaking with one of our billing experts. Call us at +1 (408) 600-0275 to learn more about how our solutions can improve your practice’s cash flow and reduce administrative burdens.
📧 Email Us
Have questions or need a customized proposal? Email us at myhealth.aiyin.us@gmail.com. We’re here to provide tailored solutions for your unique billing needs.
📍 Visit Us
We’re located at 1201 Parkmoor Ave, San Jose, CA, 95126, United States. Schedule a meeting with us to discuss how we can support your practice's financial health and operational efficiency.
Take the first step toward hassle-free medical billing—partner with My Health Aiyin and let us help your practice grow and thrive.
Are you a healthcare professional looking for reliable and efficient medical billing services? Let us help you focus on patient care while we handle your revenue cycle management with precision and compliance.
📞 Call Us Today
Get started by speaking with one of our billing experts. Call us at +1 (408) 600-0275 to learn more about how our solutions can improve your practice’s cash flow and reduce administrative burdens.
📧 Email Us
Have questions or need a customized proposal? Email us at myhealth.aiyin.us@gmail.com. We’re here to provide tailored solutions for your unique billing needs.
📍 Visit Us
We’re located at 1201 Parkmoor Ave, San Jose, CA, 95126, United States. Schedule a meeting with us to discuss how we can support your practice's financial health and operational efficiency.
Take the first step toward hassle-free medical billing—partner with My Health Aiyin and let us help your practice grow and thrive.
15
References
15
References
15
References
15
References
1. Precedence Research. (2024). U.S. Medical Billing Outsourcing Market Size, Growth, Report 2032. Retrieved from https://www.precedenceresearch.com/us-medical-billing-outsourcing-market
2. Outsource Accelerator. (2024). Why healthcare providers should outsource medical billing services. Retrieved from https://www.outsourceaccelerator.com/articles/outsource-medical-billing-services/
3. Purview Healthcare. (2024). What is Outsourcing Medical Billing: Pros & Cons Explained. Retrieved from https://purviewhealthcare.com/outsourcing-medical-billing-pros-and-cons/
4. Park Medical Billing. (2024). Advantages of Outsourcing Medical Billing vs. In-House Billers. Retrieved from https://www.parkmedicalbilling.com/advantages-of-outsourcing-medical-billing-vs-in-house-billers/
5. Global Market Insights. (2023). Medical Billing Outsourcing Market Size – Analysis Report, 2032. Retrieved from https://www.gminsights.com/industry-analysis/medical-billing-outsourcing-market
6. Fortune Business Insights. (2024). U.S. Medical Billing Outsourcing Market Size | Analysis [2030]. Retrieved from https://www.fortunebusinessinsights.com/u-s-medical-billing-outsourcing-market-109113
7. Dimension Market Research. (2024). U.S. Medical Billing Outsourcing Market Is Expected To Reach Revenue Of USD 16.9 Bn By 2033, At 12.5% CAGR. Retrieved from https://www.globenewswire.com/news-release/2024/11/19/2983846/0/en/U-S-Medical-Billing-Outsourcing-Market-Is-Expected-To-Reach-Revenue-Of-USD-16-9-Bn-By-2033-At-12-5-CAGR-Dimension-Market-Research.html
8. Outsource Strategies International. (2023). 6 Medical Billing Outsourcing Benefits for Healthcare Practices. Retrieved from https://www.outsourcestrategies.com/blog/benefits-of-outsourcing-medical-billing-services/
9. Future Market Insights. (2024). Medical Billing Outsourcing Market - Future Market Insights. Retrieved from https://www.futuremarketinsights.com/reports/medical-billing-outsourcing-market
10. IBN Technologies. (2024). 9 Benefits of Medical Billing Outsourcing. Retrieved from https://www.ibntech.com/blog/benefits-of-medical-billing-outsourcing/
11. Unity Connect. (2024). Benefits and Disadvantages of Outsourcing Medical Billing. Retrieved from https://unity-connect.com/our-resources/blog/outsourcing-medical-billing/
12. Research and Markets. (2024). U.S. Medical Billing Outsourcing Market Size & Competitors. Retrieved from https://www.researchandmarkets.com/report/united-states-medical-billing-outsourcing-market
13. Outsourcey. (2024). Top 10 Benefits of Outsourcing Medical Billing. Retrieved from https://outsourcey.com/learning-centre/top-10-benefits-of-outsourcing-medical-billing/
14. P&S Intelligence. (2024). Medical Billing Outsourcing Market Size Report, 2030. Retrieved from https://www.psmarketresearch.com/market-analysis/medical-billing-outsourcing-market-report
15. Human Medical Billing. (2024). 12 Benefits of Outsourcing Medical Billing Services for Providers. Retrieved from https://humanmedicalbilling.com/12-benefits-of-outsourcing-medical-billing-services-for-providers/
16. IMARC Group. (2024). United States Medical Billing Outsourcing Market. Retrieved from https://www.imarcgroup.com/united-states-medical-billing-outsourcing-market
17. Valerion Health. (2024). What Are The Benefits of Outsourcing Medical Billing?. Retrieved from https://valerionhealth.com/blog/benefits-of-outsourcing-medical-billing/
18. Wikipedia. (2024). Medical billing. Retrieved from https://en.wikipedia.org/wiki/Medical_billing
1. Precedence Research. (2024). U.S. Medical Billing Outsourcing Market Size, Growth, Report 2032. Retrieved from https://www.precedenceresearch.com/us-medical-billing-outsourcing-market
2. Outsource Accelerator. (2024). Why healthcare providers should outsource medical billing services. Retrieved from https://www.outsourceaccelerator.com/articles/outsource-medical-billing-services/
3. Purview Healthcare. (2024). What is Outsourcing Medical Billing: Pros & Cons Explained. Retrieved from https://purviewhealthcare.com/outsourcing-medical-billing-pros-and-cons/
4. Park Medical Billing. (2024). Advantages of Outsourcing Medical Billing vs. In-House Billers. Retrieved from https://www.parkmedicalbilling.com/advantages-of-outsourcing-medical-billing-vs-in-house-billers/
5. Global Market Insights. (2023). Medical Billing Outsourcing Market Size – Analysis Report, 2032. Retrieved from https://www.gminsights.com/industry-analysis/medical-billing-outsourcing-market
6. Fortune Business Insights. (2024). U.S. Medical Billing Outsourcing Market Size | Analysis [2030]. Retrieved from https://www.fortunebusinessinsights.com/u-s-medical-billing-outsourcing-market-109113
7. Dimension Market Research. (2024). U.S. Medical Billing Outsourcing Market Is Expected To Reach Revenue Of USD 16.9 Bn By 2033, At 12.5% CAGR. Retrieved from https://www.globenewswire.com/news-release/2024/11/19/2983846/0/en/U-S-Medical-Billing-Outsourcing-Market-Is-Expected-To-Reach-Revenue-Of-USD-16-9-Bn-By-2033-At-12-5-CAGR-Dimension-Market-Research.html
8. Outsource Strategies International. (2023). 6 Medical Billing Outsourcing Benefits for Healthcare Practices. Retrieved from https://www.outsourcestrategies.com/blog/benefits-of-outsourcing-medical-billing-services/
9. Future Market Insights. (2024). Medical Billing Outsourcing Market - Future Market Insights. Retrieved from https://www.futuremarketinsights.com/reports/medical-billing-outsourcing-market
10. IBN Technologies. (2024). 9 Benefits of Medical Billing Outsourcing. Retrieved from https://www.ibntech.com/blog/benefits-of-medical-billing-outsourcing/
11. Unity Connect. (2024). Benefits and Disadvantages of Outsourcing Medical Billing. Retrieved from https://unity-connect.com/our-resources/blog/outsourcing-medical-billing/
12. Research and Markets. (2024). U.S. Medical Billing Outsourcing Market Size & Competitors. Retrieved from https://www.researchandmarkets.com/report/united-states-medical-billing-outsourcing-market
13. Outsourcey. (2024). Top 10 Benefits of Outsourcing Medical Billing. Retrieved from https://outsourcey.com/learning-centre/top-10-benefits-of-outsourcing-medical-billing/
14. P&S Intelligence. (2024). Medical Billing Outsourcing Market Size Report, 2030. Retrieved from https://www.psmarketresearch.com/market-analysis/medical-billing-outsourcing-market-report
15. Human Medical Billing. (2024). 12 Benefits of Outsourcing Medical Billing Services for Providers. Retrieved from https://humanmedicalbilling.com/12-benefits-of-outsourcing-medical-billing-services-for-providers/
16. IMARC Group. (2024). United States Medical Billing Outsourcing Market. Retrieved from https://www.imarcgroup.com/united-states-medical-billing-outsourcing-market
17. Valerion Health. (2024). What Are The Benefits of Outsourcing Medical Billing?. Retrieved from https://valerionhealth.com/blog/benefits-of-outsourcing-medical-billing/
18. Wikipedia. (2024). Medical billing. Retrieved from https://en.wikipedia.org/wiki/Medical_billing
1. Precedence Research. (2024). U.S. Medical Billing Outsourcing Market Size, Growth, Report 2032. Retrieved from https://www.precedenceresearch.com/us-medical-billing-outsourcing-market
2. Outsource Accelerator. (2024). Why healthcare providers should outsource medical billing services. Retrieved from https://www.outsourceaccelerator.com/articles/outsource-medical-billing-services/
3. Purview Healthcare. (2024). What is Outsourcing Medical Billing: Pros & Cons Explained. Retrieved from https://purviewhealthcare.com/outsourcing-medical-billing-pros-and-cons/
4. Park Medical Billing. (2024). Advantages of Outsourcing Medical Billing vs. In-House Billers. Retrieved from https://www.parkmedicalbilling.com/advantages-of-outsourcing-medical-billing-vs-in-house-billers/
5. Global Market Insights. (2023). Medical Billing Outsourcing Market Size – Analysis Report, 2032. Retrieved from https://www.gminsights.com/industry-analysis/medical-billing-outsourcing-market
6. Fortune Business Insights. (2024). U.S. Medical Billing Outsourcing Market Size | Analysis [2030]. Retrieved from https://www.fortunebusinessinsights.com/u-s-medical-billing-outsourcing-market-109113
7. Dimension Market Research. (2024). U.S. Medical Billing Outsourcing Market Is Expected To Reach Revenue Of USD 16.9 Bn By 2033, At 12.5% CAGR. Retrieved from https://www.globenewswire.com/news-release/2024/11/19/2983846/0/en/U-S-Medical-Billing-Outsourcing-Market-Is-Expected-To-Reach-Revenue-Of-USD-16-9-Bn-By-2033-At-12-5-CAGR-Dimension-Market-Research.html
8. Outsource Strategies International. (2023). 6 Medical Billing Outsourcing Benefits for Healthcare Practices. Retrieved from https://www.outsourcestrategies.com/blog/benefits-of-outsourcing-medical-billing-services/
9. Future Market Insights. (2024). Medical Billing Outsourcing Market - Future Market Insights. Retrieved from https://www.futuremarketinsights.com/reports/medical-billing-outsourcing-market
10. IBN Technologies. (2024). 9 Benefits of Medical Billing Outsourcing. Retrieved from https://www.ibntech.com/blog/benefits-of-medical-billing-outsourcing/
11. Unity Connect. (2024). Benefits and Disadvantages of Outsourcing Medical Billing. Retrieved from https://unity-connect.com/our-resources/blog/outsourcing-medical-billing/
12. Research and Markets. (2024). U.S. Medical Billing Outsourcing Market Size & Competitors. Retrieved from https://www.researchandmarkets.com/report/united-states-medical-billing-outsourcing-market
13. Outsourcey. (2024). Top 10 Benefits of Outsourcing Medical Billing. Retrieved from https://outsourcey.com/learning-centre/top-10-benefits-of-outsourcing-medical-billing/
14. P&S Intelligence. (2024). Medical Billing Outsourcing Market Size Report, 2030. Retrieved from https://www.psmarketresearch.com/market-analysis/medical-billing-outsourcing-market-report
15. Human Medical Billing. (2024). 12 Benefits of Outsourcing Medical Billing Services for Providers. Retrieved from https://humanmedicalbilling.com/12-benefits-of-outsourcing-medical-billing-services-for-providers/
16. IMARC Group. (2024). United States Medical Billing Outsourcing Market. Retrieved from https://www.imarcgroup.com/united-states-medical-billing-outsourcing-market
17. Valerion Health. (2024). What Are The Benefits of Outsourcing Medical Billing?. Retrieved from https://valerionhealth.com/blog/benefits-of-outsourcing-medical-billing/
18. Wikipedia. (2024). Medical billing. Retrieved from https://en.wikipedia.org/wiki/Medical_billing
1. Precedence Research. (2024). U.S. Medical Billing Outsourcing Market Size, Growth, Report 2032. Retrieved from https://www.precedenceresearch.com/us-medical-billing-outsourcing-market
2. Outsource Accelerator. (2024). Why healthcare providers should outsource medical billing services. Retrieved from https://www.outsourceaccelerator.com/articles/outsource-medical-billing-services/
3. Purview Healthcare. (2024). What is Outsourcing Medical Billing: Pros & Cons Explained. Retrieved from https://purviewhealthcare.com/outsourcing-medical-billing-pros-and-cons/
4. Park Medical Billing. (2024). Advantages of Outsourcing Medical Billing vs. In-House Billers. Retrieved from https://www.parkmedicalbilling.com/advantages-of-outsourcing-medical-billing-vs-in-house-billers/
5. Global Market Insights. (2023). Medical Billing Outsourcing Market Size – Analysis Report, 2032. Retrieved from https://www.gminsights.com/industry-analysis/medical-billing-outsourcing-market
6. Fortune Business Insights. (2024). U.S. Medical Billing Outsourcing Market Size | Analysis [2030]. Retrieved from https://www.fortunebusinessinsights.com/u-s-medical-billing-outsourcing-market-109113
7. Dimension Market Research. (2024). U.S. Medical Billing Outsourcing Market Is Expected To Reach Revenue Of USD 16.9 Bn By 2033, At 12.5% CAGR. Retrieved from https://www.globenewswire.com/news-release/2024/11/19/2983846/0/en/U-S-Medical-Billing-Outsourcing-Market-Is-Expected-To-Reach-Revenue-Of-USD-16-9-Bn-By-2033-At-12-5-CAGR-Dimension-Market-Research.html
8. Outsource Strategies International. (2023). 6 Medical Billing Outsourcing Benefits for Healthcare Practices. Retrieved from https://www.outsourcestrategies.com/blog/benefits-of-outsourcing-medical-billing-services/
9. Future Market Insights. (2024). Medical Billing Outsourcing Market - Future Market Insights. Retrieved from https://www.futuremarketinsights.com/reports/medical-billing-outsourcing-market
10. IBN Technologies. (2024). 9 Benefits of Medical Billing Outsourcing. Retrieved from https://www.ibntech.com/blog/benefits-of-medical-billing-outsourcing/
11. Unity Connect. (2024). Benefits and Disadvantages of Outsourcing Medical Billing. Retrieved from https://unity-connect.com/our-resources/blog/outsourcing-medical-billing/
12. Research and Markets. (2024). U.S. Medical Billing Outsourcing Market Size & Competitors. Retrieved from https://www.researchandmarkets.com/report/united-states-medical-billing-outsourcing-market
13. Outsourcey. (2024). Top 10 Benefits of Outsourcing Medical Billing. Retrieved from https://outsourcey.com/learning-centre/top-10-benefits-of-outsourcing-medical-billing/
14. P&S Intelligence. (2024). Medical Billing Outsourcing Market Size Report, 2030. Retrieved from https://www.psmarketresearch.com/market-analysis/medical-billing-outsourcing-market-report
15. Human Medical Billing. (2024). 12 Benefits of Outsourcing Medical Billing Services for Providers. Retrieved from https://humanmedicalbilling.com/12-benefits-of-outsourcing-medical-billing-services-for-providers/
16. IMARC Group. (2024). United States Medical Billing Outsourcing Market. Retrieved from https://www.imarcgroup.com/united-states-medical-billing-outsourcing-market
17. Valerion Health. (2024). What Are The Benefits of Outsourcing Medical Billing?. Retrieved from https://valerionhealth.com/blog/benefits-of-outsourcing-medical-billing/
18. Wikipedia. (2024). Medical billing. Retrieved from https://en.wikipedia.org/wiki/Medical_billing
FAQ
How can your service reduce our administrative burden?
We already have an in-house billing team.
What makes your billing service better than others?
Your services seem expensive.
How do you handle denied claims?
We’re concerned about data security and privacy.
Can you integrate with our existing EHR system?
We’re too small to outsource our billing.
How quickly do you process claims?
We’ve had bad experiences with third-party billers before.
What is your success rate with claim approvals?
Do you provide reporting and analytics on our billing?
Our practice is unique. Can you handle our specialty-specific billing?
Can you help with patient collections?
We’re worried about the transition period.
How do you stay updated with changing billing codes and regulations?
We are a small practice and are concerned about the cost-effectiveness of your services.
Do you offer training for our staff on your billing processes?
Our current billing system seems to work fine. Why should we change?
Can you handle high volumes of billing?
We are worried about long-term contracts.
How do you handle patient billing inquiries?
We’ve heard that outsourcing billing can lead to a loss of personal touch with patients.
How can your service reduce our administrative burden?
We already have an in-house billing team.
What makes your billing service better than others?
Your services seem expensive.
How do you handle denied claims?
We’re concerned about data security and privacy.
Can you integrate with our existing EHR system?
We’re too small to outsource our billing.
How quickly do you process claims?
We’ve had bad experiences with third-party billers before.
What is your success rate with claim approvals?
Do you provide reporting and analytics on our billing?
Our practice is unique. Can you handle our specialty-specific billing?
Can you help with patient collections?
We’re worried about the transition period.
How do you stay updated with changing billing codes and regulations?
We are a small practice and are concerned about the cost-effectiveness of your services.
Do you offer training for our staff on your billing processes?
Our current billing system seems to work fine. Why should we change?
Can you handle high volumes of billing?
We are worried about long-term contracts.
How do you handle patient billing inquiries?
We’ve heard that outsourcing billing can lead to a loss of personal touch with patients.
How can your service reduce our administrative burden?
We already have an in-house billing team.
What makes your billing service better than others?
Your services seem expensive.
How do you handle denied claims?
We’re concerned about data security and privacy.
Can you integrate with our existing EHR system?
We’re too small to outsource our billing.
How quickly do you process claims?
We’ve had bad experiences with third-party billers before.
What is your success rate with claim approvals?
Do you provide reporting and analytics on our billing?
Our practice is unique. Can you handle our specialty-specific billing?
Can you help with patient collections?
We’re worried about the transition period.
How do you stay updated with changing billing codes and regulations?
We are a small practice and are concerned about the cost-effectiveness of your services.
Do you offer training for our staff on your billing processes?
Our current billing system seems to work fine. Why should we change?
Can you handle high volumes of billing?
We are worried about long-term contracts.
How do you handle patient billing inquiries?
We’ve heard that outsourcing billing can lead to a loss of personal touch with patients.
How can your service reduce our administrative burden?
We already have an in-house billing team.
What makes your billing service better than others?
Your services seem expensive.
How do you handle denied claims?
We’re concerned about data security and privacy.
Can you integrate with our existing EHR system?
We’re too small to outsource our billing.
How quickly do you process claims?
We’ve had bad experiences with third-party billers before.
What is your success rate with claim approvals?
Do you provide reporting and analytics on our billing?
Our practice is unique. Can you handle our specialty-specific billing?
Can you help with patient collections?
We’re worried about the transition period.
How do you stay updated with changing billing codes and regulations?
We are a small practice and are concerned about the cost-effectiveness of your services.
Do you offer training for our staff on your billing processes?
Our current billing system seems to work fine. Why should we change?
Can you handle high volumes of billing?
We are worried about long-term contracts.
How do you handle patient billing inquiries?
We’ve heard that outsourcing billing can lead to a loss of personal touch with patients.